Introduction
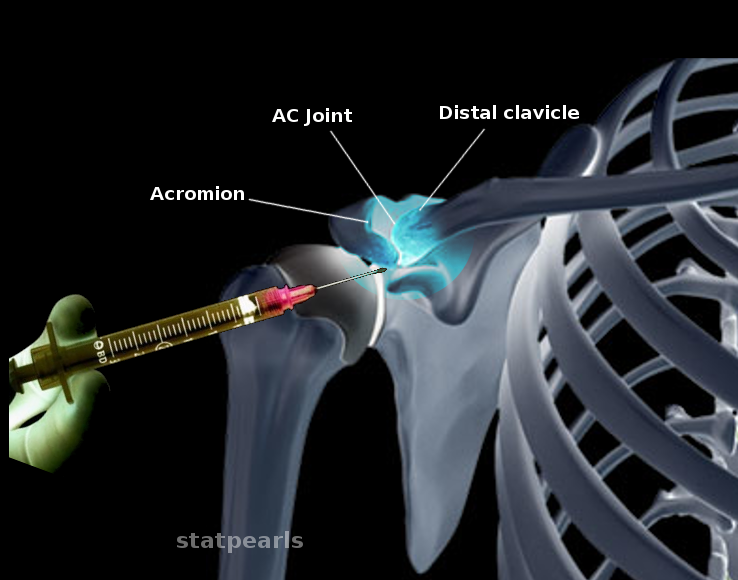
Acromioclavicular joint pathology is a common cause of shoulder pain, particularly in athletes and individuals who perform repetitive overhead activities. The acromioclavicular joint is a synovial joint at the acromion process of the scapula and the clavicle (see Image. Acromioclavicular Joint Injection). The acromioclavicular joint is designed with limited mobility but significant load-bearing responsibility, especially during arm elevation.
The etiology of acromioclavicular joint pathology is often multifactorial, stemming from degenerative changes, inflammatory processes, repetitive mechanical stress, or traumatic injury.[1][2] Degenerative changes common to the acromioclavicular joint due to osteoarthritis include joint space narrowing, cartilage wear, and osteophyte formation. Inflammatory arthritis, including rheumatoid arthritis, may also affect the acromioclavicular joint. Repetitive mechanical stress can also cause bony or soft tissue injury and degeneration. Acute trauma to the acromioclavicular joint can cause bony or ligamentous injuries. Acromioclavicular sprains can result in a hypermobile and unstable acromioclavicular joint, increasing the likelihood of developing arthritic changes.
Acromioclavicular joint injections serve diagnostic and therapeutic purposes in managing acromioclavicular joint pain. Diagnostic injections involve administering an anesthetic, where pain relief confirms the source of the pain. Diagnostic injections can be used in presurgical evaluations to identify candidates for procedures such as distal clavicle excision.[3] Therapeutically, corticosteroid, hyaluronic acid, or platelet-rich plasma injections are used to reduce pain and improve function.[4] These injections are especially valuable for patients who have not responded adequately to conservative treatments such as physical therapy, nonsteroidal anti-inflammatory drugs, or activity modification. Hyaluronic acid and platelet-rich plasma injections have shown questionable benefits in knee osteoarthritis, and there is a lack of high-quality studies supporting their use for AC joint osteoarthritis.[5]
Results of acromioclavicular injection can vary depending on the pathology and injection composition. Corticosteroid injections often provide significant pain relief, though the effect is typically temporary, lasting from weeks to months.[6][7][8] Corticosteroid injections are appropriate for patients seeking short-term relief, such as athletes aiming to return to activity or to enable more efficient progress in rehabilitation programs designed to restore shoulder mobility and strength. Therapeutic injections can be repeated as necessary; however, evidence indicates diminishing effectiveness with frequent use, particularly in cases of advanced joint degeneration.[4]
Various techniques are used to administer acromioclavicular joint injections. Conventional landmark-guided injections rely on palpating anatomical landmarks for injection site location. Landmark-guided injections are commonly used due to their simplicity and minimal resource requirements. Unfortunately, this method often results in medication being delivered outside the joint space due to improper injection site identification.
Imaging-guided techniques such as fluoroscopy and ultrasound can be used with superior precision.[9][10] Ultrasound guidance is increasingly preferred to fluoroscopy as it is noninvasive, costs less, and enables improved outcomes due to the real-time visualization of needle placement. Study results have shown that ultrasound-guided injections improve accuracy rates significantly and reduce the risk of procedural complications.[11]
Additionally, ultrasound guidance reduces patient discomfort, as the clinician can more confidently and precisely deliver the injection to the target area.[12] Outcomes improve when injections are integrated with comprehensive rehabilitation programs rather than as a standalone treatment.[13] As with other interventions, patient selection, accurate delivery, and integrating injections within a broader management plan are critical to achieving optimal outcomes.
Anatomy and Physiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Anatomy and Physiology
The acromioclavicular joint is a planar, diarthroidal synovial joint located at the junction of the acromion process of the scapula and the distal clavicle. This joint plays a pivotal role in shoulder function by stabilizing the scapula superiorly and maintaining joint alignment during arm elevation. The structure of the acromioclavicular joint includes a fibrocartilaginous disc, a joint capsule, and surrounding ligaments (acromioclavicular, coracoclavicular, and coracoacromial), which provide structural integrity to the acromioclavicular joint and facilitate load transmission between the clavicle and scapula.
Capsular ligaments surround the acromioclavicular joint to provide stability superiorly, inferiorly, posteriorly, and anteriorly.[14] The conoid and trapezoid ligaments, which comprise the coracoclavicular ligament, span the distance between the superior surface of the coracoid to the conoid tuberosity and trapezoid ridge of the clavicle. The coracoclavicular ligament prevents vertical displacement of the acromioclavicular joint. The deltoid and trapezius muscles afford dynamic stability to the acromioclavicular joint during clavicular and scapular motion.[15]
The acromioclavicular joint's small size and superficial location heighten the risk of needle misplacement with landmark-guided techniques. Additionally, the joint's narrow space and intricate ligamentous attachments further complicate accurate needle placement. The proximity of the joint to neurovascular structures, such as the supraclavicular nerve, heightens the risk of nerve irritation or injury during injection.[16]
Acromioclavicular joint disease commonly arises from degenerative, traumatic, or inflammatory processes. Degenerative changes, particularly osteoarthritis, are prevalent in athletes and laborers who engage in repetitive overhead activities that stress the joint, leading to cartilage erosion, joint space narrowing, and osteophyte formation. Traumatic injuries can sprain or tear the ligaments of the acromioclavicular joint, resulting in instability and promoting arthritic changes over time. Also, rheumatoid arthritis can inflame the synovium, causing joint swelling, pain, and reduced range of motion. A recent systematic review showed that 13% to 95% of adults exhibit radiographic evidence of degenerative arthritis in the acromioclavicular joint.[17]
Indications
Acromioclavicular joint injections function diagnostically, confirming the source of pain and therapeutically providing symptom relief to enhance patient comfort and functional ability.[8] Intraarticular acromioclavicular injections have produced promising short-term outcomes, but studies evaluating mid-term to long-term results of intraarticular acromioclavicular injections are scarce. Results from prior studies have demonstrated positive short-term outcomes for pain relief and shoulder function at a maximum follow-up of 3 weeks.[18] Hossain et al reported significant pain relief for at least 12 months after treatment with a single acromioclavicular injection, while van Riet et al found that only 28% of patients treated with acromioclavicular injection experienced significant benefits in shoulder function and pain relief 1 month after injection.[4][7]
Diagnostic acromioclavicular joint injections can help assess anterior shoulder pain, especially when clinical evaluation and imaging provide inconclusive findings. Symptoms of acromioclavicular joint pathology often include localized tenderness, pain during overhead or cross-body movements, and limited shoulder range of motion. A diagnostic injection with a local anesthetic can help confirm the acromioclavicular joint as the primary pain source, which is particularly useful when considering surgical options.
Therapeutic indications for acromioclavicular joint injections include pain management for conditions like osteoarthritis, inflammatory arthritis, and chronic post-traumatic changes.[8] For patients with osteoarthritis, corticosteroids, hyaluronic acid, and platelet-rich plasma injections can reduce pain and enhance function. They are typically used when conservative treatments like physical therapy, nonsteroidal anti-inflammatory drugs, or lifestyle changes are ineffective. Chronic overuse or traumatic injuries, frequently seen in athletes and laborers, may benefit from corticosteroid injections to control ongoing inflammation and aid in rehabilitation aimed at restoring shoulder mechanics.
Contraindications
Contraindications for acromioclavicular joint injections include fractures or active infections at the injection site, systemic infections, and hypersensitivity or significant allergic reactions to corticosteroids or local anesthetics. Careful consideration is required for patients with coagulopathy or those receiving anticoagulant therapy, as these conditions increase the risk of bleeding. Additionally, individuals with poorly controlled diabetes warrant caution because corticosteroids can significantly elevate blood glucose levels. Repeated injections in close succession should be avoided to reduce the risk of joint degradation and potential long-term complications, such as cartilage damage or chronic instability.
Equipment
Equipment Needed for Acromioclavicular Joint Injections
The following are used for this procedure:
- Skin antiseptics such as alcohol, betadine, or chlorhexidine
- Sterile gloves, drapes, and 10 cc syringes
- Standard 5/8 or 1.5 inch; 25 or 27 gauge needles
- For ultrasound-guided injections: sterile ultrasound probe covers and ultrasound gel
- For fluoroscopic-guided injections: protective lead aprons and contrast solution
Injectable Options
- Local anesthetics such as lidocaine, ropivacaine, or bupivacaine
- Corticosteroids such as methylprednisolone acetate, triamcinolone acetate, betamethasone acetate, betamethasone phosphate, or dexamethasone phosphate
- Sodium hyaluronate
- Platelet-rich plasma
Adjust the volume and dose according to the patient's body size, comorbidities, and joint size. When combining local anesthetics with corticosteroids or other injectables, ensure compatibility and adhere to recommended dosage limits to avoid overdosage. The AC joint can typically take no more than 2 mL of injectate.
Local Anesthetic Dosing Suggestions for Acromioclavicular Joint Injections
-
Lidocaine
- Concentration: 1% or 2%
- Dose: 1 to 2 mL (maximum single dose: 300 mg for 1%; 600 mg for 2%, depending on patient size and comorbidities)
- Duration of action: 1 to 2 hours
-
Bupivacaine
- Concentration: 0.25% or 0.5%
- Dose: 1 to 2 mL (maximum single dose: 175 mg for bupivacaine only; 225 mg if mixed with epinephrine)
- Duration of action: 4 to 6 hours for 0.25%; up to 8 hours for 0.5%
Corticosteroids Dosing Suggestions for Acromioclavicular Joint Injections
-
Methylprednisolone acetate (depo-medrol)
- Dose: 20 to 40 mg
- Volume: typically mixed with 0.5 to 1 mL of local anesthetic
- Onset/duration: 24 to 48 hours for onset; lasts weeks to months
-
Triamcinolone acetonide (Kenalog)
- Dose: 10 to 40 mg
- Volume: usually combined with 0.5 to 1 mL of local anesthetic
- Onset/duration: 24 to 48 hours for onset; lasts weeks to months
-
Betamethasone acetate/betamethasone sodium phosphate (celestone soluspan)
- Dose: 6 to 12 mg (total for combination preparation)
- Volume: mixed with 0.5 to 1 mL of local anesthetic
- Onset/duration: rapid onset (hours); lasts weeks to months
-
Dexamethasone sodium phosphate
- Dose: 4 to 8 mg
- Volume: usually mixed with 0.5 to 1 mL of local anesthetic
- Onset/duration: onset within hours; lasts 1 to 2 weeks (shortest duration of corticosteroids)
Personnel
The procedural team typically includes a clinician experienced in acromioclavicular joint injections, a nurse or medical assistant, and an operator skilled in using a fluoroscopic C-arm or ultrasound. For platelet-rich plasma (PRP) therapy cases, personnel trained in PRP processing systems may also be required to prepare the sample before injection. All team members should be proficient in managing potential complications associated with the procedure to ensure patient safety and optimal outcomes.
Preparation
The risks and benefits of the procedure should be thoroughly discussed with the patient. Informed consent must be obtained per institutional policies. Before the injection, a time-out should be performed to verify the patient’s identity and the correct injection site. The patient should be seated or semi-reclined on the examination table. After identifying the injection site, it should be marked, cleansed with a skin antiseptic solution, and covered with sterile drapes.
PRP injections start by drawing 15 to 60 mL of the patient’s blood, depending on the required volume and concentration of PRP. The blood is placed in a centrifuge, which separates platelets and plasma from other components, creating a concentrated platelet-rich plasma layer. The PRP layer is carefully extracted following centrifugation to preserve platelet integrity and minimize dilution with other blood elements. The prepared PRP is subsequently drawn into a syringe, making it ready for injection.
Technique or Treatment
Landmark-Guided Injection
-
Site preparation
- Identify the acromioclavicular joint by palpating the clavicle distally until its endpoint. Palpate the small depression just lateral to the termination of the clavicle, which is the joint space.
- Clean the injection site thoroughly with an antiseptic solution.
- Optional: Use a skin marker to mark the injection site directly over the acromioclavicular joint line for accurate needle placement.
-
Injection preparation
- Prepare the syringe with the injectable chosen for the procedure (analgesic, corticosteroid, sodium hyaluronate, or PRP).
- Attach a 25- or 27-gauge needle to the syringe.
-
Injection technique
- Insert the needle perpendicular to the skin and directly into the acromioclavicular joint space. Angling the needle slightly toward the distal clavicle can be helpful.
- Advance slowly, feeling for a reduction in resistance as the needle enters the joint space.
- Aspirate to confirm that there is no blood return before injection.
- Inject the medication slowly into the joint.
-
Post-injection care
- Remove the needle, apply gentle pressure to the site to prevent bleeding, and cover with a sterile bandage.
Ultrasound-Guided Injection
-
Injection site and ultrasound preparation
- Set up the ultrasound machine and select a high-frequency linear transducer (10 to 15 MHz) to visualize the superficial acromioclavicular joint.
- Identify the acromioclavicular joint on ultrasound by locating the bony landmarks of the distal clavicle and acromion and confirming the joint space.
- Clean the skin with an antiseptic solution and apply sterile ultrasound gel to the injection site. Place the probe in a sterile cover to maintain a sterile field.
-
Injection preparation
- Prepare a syringe with the injectable chosen for the procedure (analgesic, corticosteroid, sodium hyaluronate, PRP).
- Attach a 25- or 27-gauge needle.
-
Injection technique
- Using the ultrasound probe, locate the acromioclavicular joint in a transverse or longitudinal view, confirming the joint space and needle pathway.
- Insert the needle using an in-plane or out-of-plane technique, advancing slowly toward the acromioclavicular joint space under ultrasound guidance.
- Observe the needle's position in real time, ensuring entry into the joint capsule.
- Once the needle is within the joint, aspirate to confirm no blood return, then inject the medication slowly, visualizing the solution and filling the joint space on an ultrasound.
-
Post-injection care
- Remove the needle, apply gentle pressure to the site to prevent bleeding, and cover with a sterile bandage.
Fluoroscopic-Guided Injection
-
Site preparation
- Palpate the acromioclavicular joint by identifying the bony landmarks of the distal clavicle and acromion.
- Clean the injection site with an antiseptic solution such as chlorhexidine or iodine, and mark the injection entry point over the acromioclavicular joint line.
- Prepare the fluoroscopic unit, positioning it to achieve an optimal anterior-posterior view of the acromioclavicular joint.
-
Injection preparation
- Prepare the syringe with the injectable chosen for the procedure (analgesic, corticosteroid, sodium hyaluronate, or PRP).
- Attach a 25- or 27-gauge needle to the syringe.
-
Injection technique
- Position the needle perpendicular to the skin, aligned with the fluoroscopic anterior-posterior view of the acromioclavicular joint.
- Insert the needle toward the joint space, adjusting the fluoroscope to maintain optimal visualization of the needle’s path.
- Once the needle is near the joint, inject a small amount of contrast dye under fluoroscopy to confirm accurate placement within the joint space.
- After confirming proper placement, inject the prepared medication into the joint.
-
Post-injection care
- Withdraw the needle, apply pressure to prevent bleeding, and place a sterile bandage over the site.
Complications
Although rare, possible complications of acromioclavicular joint injections include:
- Infection
- Bleeding or hematoma formation
- Allergic reaction
- Post injection pain
- Joint degradation
- Tendon or ligament damage
- Neurovascular injury
Complications associated with corticosteroid injections include:
- Skin and soft tissue atrophy
- Hypopigmentation
- Tendon weakening or rupture
- Joint cartilage damage
- Elevated blood glucose levels (especially in patients with diabetes)
- Systemic effects such as facial flushing, mood changes, insomnia, and increased blood pressure
Complications associated with hyaluronic acid injections include:
- Joint effusion
- Skin reactions
- Stiffness or decreased range of motion
- Synovitis
- Systemic reactions such as headaches or nausea
- Infection or foreign body reaction
Complications associated with PRP injections include:
- Calcification within the injected tissue
- Joint effusion
Clinical Significance
Acromioclavicular joint injections provide diagnostic and therapeutic benefits in managing acromioclavicular joint pathology. These injections are commonly utilized to confirm the diagnosis of acromioclavicular joint disorders and to alleviate symptoms associated with inflammation or degenerative changes in the joint.
Diagnostic Benefit of Acromioclavicular Joint Injections
The primary diagnostic purpose of acromioclavicular joint injections is to determine whether the acromioclavicular joint is the source of shoulder pain. This is achieved by injecting a local anesthetic, with or without a corticosteroid, into the joint. Significant pain relief following the injection confirms the joint's involvement, helping differentiate it from other potential causes of shoulder pain, such as rotator cuff pathology.
Therapeutic Benefit of Acromioclavicular Joint Injections
Acromioclavicular joint injections are also used therapeutically to reduce inflammation and provide symptomatic relief for conditions such as osteoarthritis, traumatic injuries, or inflammatory conditions of the joint. The corticosteroid component of the injection can reduce inflammation and pain, thereby improving function and quality of life. In some instances, repeated injections may be required to sustain symptom relief. These injections are typically part of a comprehensive management plan that may also include physical therapy or, in more severe instances—surgical intervention.
Enhancing Healthcare Team Outcomes
The interprofessional team ensures patient safety and optimizes outcomes during acromioclavicular joint injections. Advanced clinicians take the lead in diagnosing acromioclavicular joint pathology, selecting suitable candidates for injection, and performing the procedure, often with imaging guidance for precision. Nurses support by ensuring patient comfort, preparing the injection site with sterile techniques to prevent infection, and educating patients on post-procedure care and monitoring for adverse effects.
Pharmacists review medications for potential contraindications, such as anticoagulants or allergies, and guide appropriate corticosteroid dosing to minimize systemic risks. Physical therapists contribute by designing rehabilitation programs to reduce pain, enhance shoulder range of motion, and restore functional strength, fostering long-term shoulder health. This collaborative approach, paired with comprehensive patient education and close monitoring, maximizes the therapeutic benefits of acromioclavicular joint injections while minimizing risks and complications.
Media
(Click Image to Enlarge)
References
Shaffer BS. Painful conditions of the acromioclavicular joint. The Journal of the American Academy of Orthopaedic Surgeons. 1999 May-Jun:7(3):176-88 [PubMed PMID: 10346826]
Petersson CJ. The acromioclavicular joint in rheumatoid arthritis. Clinical orthopaedics and related research. 1987 Oct:(223):86-93 [PubMed PMID: 3652595]
Tallia AF, Cardone DA. Diagnostic and therapeutic injection of the shoulder region. American family physician. 2003 Mar 15:67(6):1271-8 [PubMed PMID: 12674455]
Hossain S, Jacobs LG, Hashmi R. The long-term effectiveness of steroid injections in primary acromioclavicular joint arthritis: a five-year prospective study. Journal of shoulder and elbow surgery. 2008 Jul-Aug:17(4):535-8. doi: 10.1016/j.jse.2007.12.001. Epub 2008 Mar 24 [PubMed PMID: 18359647]
Du D, Liang Y. A meta-analysis and systematic review of the clinical efficacy and safety of platelet-rich plasma combined with hyaluronic acid (PRP + HA) versus PRP monotherapy for knee osteoarthritis (KOA). Journal of orthopaedic surgery and research. 2025 Jan 17:20(1):57. doi: 10.1186/s13018-024-05429-w. Epub 2025 Jan 17 [PubMed PMID: 39819683]
Level 1 (high-level) evidenceJacob AK, Sallay PI. Therapeutic efficacy of corticosteroid injections in the acromioclavicular joint. Biomedical sciences instrumentation. 1997:34():380-5 [PubMed PMID: 9603070]
van Riet RP, Goehre T, Bell SN. The long term effect of an intra-articular injection of corticosteroids in the acromioclavicular joint. Journal of shoulder and elbow surgery. 2012 Mar:21(3):376-9. doi: 10.1016/j.jse.2011.05.010. Epub 2011 Jun 22 [PubMed PMID: 21700479]
Welch M, Rankin S, How Saw Keng M, Woods D. A systematic review of the treatment of primary acromioclavicular joint osteoarthritis. Shoulder & elbow. 2024 Apr:16(2):129-144. doi: 10.1177/17585732231157090. Epub 2023 Feb 22 [PubMed PMID: 38655415]
Level 1 (high-level) evidencePeck E, Lai JK, Pawlina W, Smith J. Accuracy of ultrasound-guided versus palpation-guided acromioclavicular joint injections: a cadaveric study. PM & R : the journal of injury, function, and rehabilitation. 2010 Sep:2(9):817-21. doi: 10.1016/j.pmrj.2010.06.009. Epub [PubMed PMID: 20869680]
Bisbinas I, Belthur M, Said HG, Green M, Learmonth DJ. Accuracy of needle placement in ACJ injections. Knee surgery, sports traumatology, arthroscopy : official journal of the ESSKA. 2006 Aug:14(8):762-5 [PubMed PMID: 16465536]
Edelson G, Saffuri H, Obid E, Lipovsky E, Ben-David D. Successful injection of the acromioclavicular joint with use of ultrasound: anatomy, technique, and follow-up. Journal of shoulder and elbow surgery. 2014 Oct:23(10):e243-50. doi: 10.1016/j.jse.2014.01.012. Epub 2014 Apr 13 [PubMed PMID: 24725899]
Park KD, Kim TK, Lee J, Lee WY, Ahn JK, Park Y. Palpation Versus Ultrasound-Guided Acromioclavicular Joint Intra-articular Corticosteroid Injections: A Retrospective Comparative Clinical Study. Pain physician. 2015 Jul-Aug:18(4):333-41 [PubMed PMID: 26218936]
Level 2 (mid-level) evidenceHarris KD, Deyle GD, Gill NW, Howes RR. Manual physical therapy for injection-confirmed nonacute acromioclavicular joint pain. The Journal of orthopaedic and sports physical therapy. 2012 Feb:42(2):66-80. doi: 10.2519/jospt.2012.3866. Epub 2011 Oct 25 [PubMed PMID: 22030329]
Lervick GN. Direct arthroscopic distal clavicle resection: a technical review. The Iowa orthopaedic journal. 2005:25():149-56 [PubMed PMID: 16089089]
Flores DV, Goes PK, Gómez CM, Umpire DF, Pathria MN. Imaging of the Acromioclavicular Joint: Anatomy, Function, Pathologic Features, and Treatment. Radiographics : a review publication of the Radiological Society of North America, Inc. 2020 Sep-Oct:40(5):1355-1382. doi: 10.1148/rg.2020200039. Epub 2020 Aug 7 [PubMed PMID: 32762593]
Borbas P, Eid K, Ek ET, Feigl G. Innervation of the acromioclavicular joint by the suprascapular nerve. Shoulder & elbow. 2020 Jun:12(3):178-183. doi: 10.1177/1758573219851005. Epub 2019 May 20 [PubMed PMID: 32565919]
Ibounig T, Rämö L, Haas R, Jones M, Järvinen TLN, Taimela S, Docking S, Sanders S, Buchbinder R. Imaging abnormalities of the acromioclavicular joint and subacromial space are common in asymptomatic shoulders: a systematic review. Journal of orthopaedic surgery and research. 2025 Jan 3:20(1):7. doi: 10.1186/s13018-024-05378-4. Epub 2025 Jan 3 [PubMed PMID: 39754140]
Level 1 (high-level) evidenceKurta I, Datir S, Dove M, Rahmatalla A, Wynn-Jones C, Maffulli N. The short term effects of a single corticosteroid injection on the range of motion of the shoulder in patients with isolated acromioclavicular joint arthropathy. Acta orthopaedica Belgica. 2005 Dec:71(6):656-61 [PubMed PMID: 16459853]