Introduction
Duret hemorrhages are small, linear, or flame-shaped brainstem hemorrhages that occur due to transtentorial herniation involving the midbrain and upper pons. First described by the French neurologist Henri Duret, these hemorrhages result from vascular compromise due to downward displacement of the brainstem that leads to stretching and tearing of perforating arteries, particularly the paramedian branches of the basilar artery. Brainstem hemorrhages are broadly classified as primary or secondary. Primary hemorrhages arise from direct trauma, hypertension, or coagulopathy, compared to secondary hemorrhages, such as Duret hemorrhages, that occur due to descending transtentorial herniation from various etiologies.[1]
Studies on brain trauma by Duret localized autonomic disturbances to the brainstem and linked them to microhemorrhages in the pons and medulla.[2] While historically considered a postmortem finding, advances in neuroimaging have enabled antemortem diagnosis of these hemorrhages, highlighting the importance of their early recognition in those who are critically ill. Given their association with devastating neurological injury, Duret hemorrhages signify an urgent need for aggressive management of intracranial hypertension and herniation syndromes. This course analyzes the pathophysiology, imaging characteristics, clinical implications, and management strategies associated with Duret hemorrhages.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
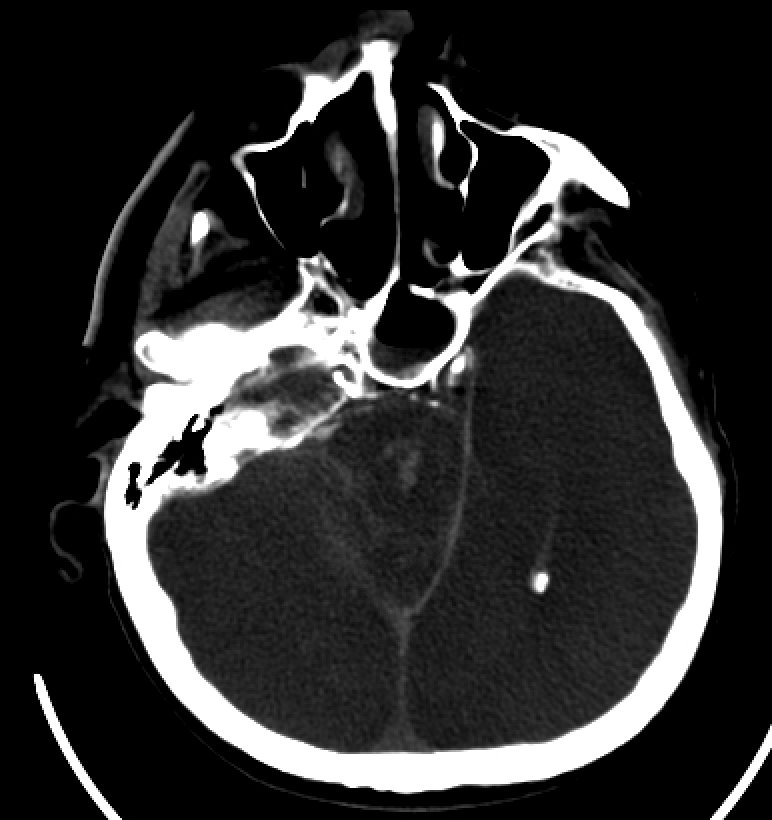
Duret hemorrhages are small sites of bleeding in the brainstem due to descending transtentorial herniation, which occurs with increased intracranial pressure (ICP) and resultant intracranial compartmental brain shifts (see Image. Duret Hemorrhage, Computed Tomography Scan). The most common causes of these hemorrhages include traumatic brain injury (TBI), subdural and epidural hematoma development, intraparenchymal hemorrhage, acute diffuse cerebral edema, brain neoplasms, hyponatremia, and the rare administration of thrombolytic therapy.[3][4][5][6][7] While typically associated with increased ICP, Duret hemorrhages have also been reported in a few cases resulting from intracranial hypotension.[8][9]
Duret hemorrhages develop when significant mass effect from cerebral edema, intracranial hematomas, or brain tumors causes brain tissue to shift from its normal anatomical position, resulting in uncal or transtentorial herniation. This downward displacement of the brainstem stretches and tears the penetrating arteries that supply the midbrain and pons, in particular the paramedian branches of the basilar artery. This vascular compromise leads to hemorrhagic infarction of the midline, paramedian, and ventral regions of the tegmentum of the upper pons and midbrain. Direct mechanical damage, disruption of blood flow, and sustained increase in ICP further exacerbate the brainstem injury. Duret hemorrhages represent a critical indication of severe brain injury and often indicate a poor prognosis. Their presence signifies impending brainstem compromise and is often associated with irreversible neurological damage.
Epidemiology
The precise epidemiology of Duret hemorrhages is not widely documented because they are usually found on postmortem examination in cases of severe brain injury. These hemorrhages occur due to conditions that result in brain herniation, such as large intracranial hematomas, severe TBI, or brain tumors.[10] Since Duret hemorrhages are often a marker of irreversible brainstem injury, the condition is rarely diagnosed in patients who survive, and their true prevalence remains uncertain.
The incidence of Duret hemorrhages varies significantly between neuropathological and radiological studies. Autopsy-based studies report an incidence of 30% to 60% compared to radiological studies that estimate a much lower occurrence rate of 5% to 10%.[1] This discrepancy may be explained by the fact that up to 20% of secondary brainstem hemorrhages occur at the microscopic level, which makes them undetectable on conventional imaging. Additionally, there may be a delay in developing the Duret hemorrhages, which indicates that the initial computed tomography scans may not demonstrate their presence. Risk factors associated with the development of Duret hemorrhages include arterial hypertension and advanced age, both of which may contribute to increased vascular fragility and a susceptibility to hemorrhagic infarction.[1]
Pathophysiology
Most clinicians believe that the hypothesis underlying Duret hemorrhage is related to the distortion of the pontine perforating arterial branches that extend from the relatively immobile basilar artery due to the caudal displacement of the upper brainstem, due to descending transtentorial herniation, which is coupled with an anterior-posterior elongation of the brainstem from the side-to-side compression. However, some authors have also postulated that there may be a venous origin of these hemorrhages due to obstruction of the venous return that results from a sudden increase in ICP, which results in venous thrombosis, infarction, and hemorrhage.[2][11]
Duret hemorrhages represent bleeding in the midbrain and pons of the brainstem that is usually seen in cases of severe brain trauma or other conditions causing increased ICP. Here is a brief overview of the pathophysiology:
- Increased ICP
- Conditions such as TBI, brain tumors, large intracranial hematomas, or brain edema can cause a significant increase in ICP.
- Brain herniation
- The increased ICP can cause parts of the brain to shift from their normal position in a process known as herniation.[12] Specifically, uncal or transtentorial herniation can result where the medial temporal lobe is pushed against the brainstem or through the tentorial notch.
- Impaired blood flow
- This abnormal ICP and movement of the brainstem can compress or stretch the small, penetrating arteries that supply the brainstem, which prevents blood flow to those areas.
- Ischemic injury and hemorrhage
- Reduced or absent blood flow to the brainstem can cause ischemic injury to brain tissue. This vascular damage makes the blood vessels in that area more susceptible to rupture, which results in hemorrhage.
- Duret hemorrhages
- These areas of hemorrhage in the midbrain and pons are associated with the decreased blood flow to the brainstem and the resultant ischemic injury caused by the herniation process.
Duret hemorrhages are usually a secondary event that occurs after a significant brain injury or in the presence of increased ICP, where they indicate severe brain damage with a poor prognosis. They are most often identified postmortem at the time of the autopsy.
Histopathology
In the 18th century, Henri Duret confirmed that trauma resulted in variations in cerebrospinal fluid distribution that caused changes in the ICP in the spaces where the fluid circulates, such as the cerebral aqueduct. Duret noted microhemorrhages in the brainstem and the surrounding tissue as “action of a pressure increases in the cerebrospinal fluid due to sudden accumulation, which caused a linear hemorrhage on the medulla’s thickness and around the central canal.”[1] Histopathologically, Duret hemorrhages are characterized by small, linear areas of bleeding in the midbrain and pons of the brainstem. They are usually associated with severe brain injury, such as transtentorial herniation.
Upon microscopic examination, those findings may represent:
- Acute hemorrhage
- In the acute phase, red blood cells and hemorrhagic necrosis of the surrounding brain tissue may be evident.
- Chronic lesions
- If the person survives after the hemorrhage, the lesion may evolve. Over time, the hemorrhage may become organized, with macrophages infiltrating into the area to clear the dead tissue. In the later stages, gliosis, a process where glial cells proliferate to form a glial scar, may occur.
- Vascular disruption
- There may be evidence of disruption to the small, penetrating arteries of the brainstem that represent the underlying cause of the Duret hemorrhages.
- Associated findings
- Because Duret hemorrhages are usually associated with significant brain herniation, there may also be histopathological findings such as neuronal injury or necrosis in other areas of the brain that have been affected by the herniation.
These histopathological features will depend on the time of the analysis and the severity of the brain injury. As Duret hemorrhages typically indicate severe brain damage and have a poor prognosis, they are often identified postmortem during an autopsy.[12]
History and Physical
In most cases of Duret hemorrhage, there is a prior history of head trauma, brain tumor, or another space-occupying lesion. Often, the patient may have an altered sensorium ranging from confusion to a comatose state associated with underlying transtentorial herniation and the disruption of the reticular activating system. There is often anisocoria due to the involvement of the ipsilateral third cranial nerve with contralateral motor weakness.
In some cases, ipsilateral weakness can present due to the “Kernohan notch” phenomenon, where there is compression of the cerebral peduncle on the contralateral side of the brainstem against the tentorium cerebelli.[13] With downward transtentorial herniation, the patient can demonstrate progression from decorticate to decerebrate posturing with the loss of brainstem reflexes and alteration in the respiratory pattern from Cheyne-Stokes to ataxic breathing. With the upward transtentorial herniation that results following cerebral spinal fluid diversion procedures, there may be an associated Perinaud syndrome.[14][15]
Evaluation
The initial evaluation of the patient requires a computed tomography (CT) scan of the head to discern whether there are supratentorial and infratentorial abnormalities, such as brain tumors with vasogenic edema causing mass effect or epidural, subdural, or intraparenchymal hemorrhage. Central herniation results in complete obliteration of the perimesencephalic and perimedullary cisterns with or without small hemorrhages in the midline, paramedian, and ventral regions in the tegmentum of the upper pons and midbrain (see Image. Computed Tomography Scan of a Duret Hemorrhage). The posterior cerebral artery may occasionally be kinked at the tentorial edge, resulting in occipital lobe infarction. Required laboratory investigations include a serum sodium level, arterial blood gases, and a basic metabolic profile.
Treatment / Management
First and foremost, the airway, breathing, and circulation of the patient should be addressed. An emergent noncontrast CT scan of the head should be obtained, followed by the aggressive treatment of the intracranial hypertension if it is present on the scan. Identification of the underlying cause of the elevated ICP, with the timely management of the cause, represents the therapeutic course of action for the patient. The necessary basic labs include blood count, metabolic panel, and coagulation profile. If the clinician establishes that trauma is the cause of epidural or subdural hemorrhage leading to herniation, then the rapid surgical evacuation of the hematoma should be pursued.[16](A1)
Steps for managing increased intracranial hypertension include:
- Raising the head of the bed by 30 to 60 degrees.
- Hyperventilation may be needed to keep the PaCo2 (partial pressure of carbon dioxide) between 30 and 35 mm Hg.
- Osmolar therapy that includes hypertonic saline and/or mannitol therapy can help manage the pressure.
- ICP monitoring and keeping the ICP <20 mm Hg may be necessary.
- In cases of brain tumors and associated vasogenic edema, dexamethasone might help reduce the mass effect caused by the tumor.
- Surgical interventions (eg, decompression of mass/hematoma) may also be warranted.
The clinical goal in the intensive care unit is to maintain normotension, normovolemia, normonatremia to hypernatremia, normoglycemia, and normothermia to hypothermia. Such patients are followed with serial neurological examinations and head CT scans in the intensive care unit.
Differential Diagnosis
The most common differential diagnosis includes primary brainstem hemorrhages, which are petechial in appearance and represent hypertensive bleeds. Radiologically, Duret hemorrhages have a linear configuration that extends in the brainstem from a ventral and dorsal location, but may be of any shape in the clinical setting of supratentorial abnormalities that cause transtentorial herniation. Primary hypertensive hemorrhages are usually larger and occur spontaneously in patients with an antecedent history of uncontrolled hypertension without supratentorial abnormalities. Petechial hemorrhages are multifocal and small in size and are seen around the dorsal midbrain in periaqueductal and tectal locations in cases with diffuse axonal injuries following TBI.[17]
Prognosis
The presence of Duret hemorrhages has invariably been regarded as a poor prognostic sign. However, increasing case report numbers suggest functional recovery may be possible after a Duret hemorrhage.[18] The presence of a Duret hemorrhage alone should in itself not be considered a poor prognostic indicator and should not by itself result in the decision to withdraw care.[19] Depending on the underlying cause of the transtentorial herniation, there have been a few case reports that resulted in a good prognosis in patients with severe hyponatremia, subdural hemorrhage, and TBI.[20][21][22] The direct correlation between recovery and the rapid reversibility of the underlying cause remains uncertain.
Complications
Duret hemorrhages are typically associated with severe brain injury and carry a poor prognosis due to their location in the brainstem, which contains critical autonomic and motor functions. The most significant complications arise from direct damage to the midbrain and pons, leading to devastating neurological deficits. Patients may develop loss of consciousness, coma, and ultimately, brain death due to disruption of the reticular activating system. Respiratory failure is common, as the brainstem regulates this vital autonomic function.
Motor dysfunction is another major complication of Duret hemorrhage, often presenting as quadriplegia due to corticospinal tract involvement. Cranial nerve deficits may occur with abnormalities in the pupillary response, ocular movement, and ability to swallow. Patients who survive the acute phase of the injury may experience persistent neurological impairment that includes spasticity, dysphagia, and the locked-in syndrome. Additionally, the severe elevation in ICP associated with Duret hemorrhages increases the risk of secondary ischemia and further brain injury. Due to the often fatal nature of these hemorrhages, survivors typically require prolonged intensive care, mechanical ventilation, and rehabilitative support.
Deterrence and Patient Education
Deterrence of Duret hemorrhages is primarily associated with the prevention and early management of conditions that lead to increased ICP and brain herniation. Prompt recognition and treatment of intracranial hemorrhages, TBIs, brain tumors, and other causes of elevated ICP can reduce the risk of transtentorial herniation and the subsequent development of brainstem hemorrhages. Optimizing blood pressure management, particularly in hypertensive individuals, is essential because arterial hypertension has been identified as a risk factor for Duret hemorrhages. Careful monitoring and timely neurosurgical intervention in patients with expanding intracranial hematomas or severe cerebral edema can prevent secondary brainstem injury.
Patient and caregiver education should emphasize the importance of seeking immediate medical attention for symptoms of increased ICP, such as severe headache, altered mental status, vomiting, and focal neurological deficits. Public awareness campaigns about TBI prevention, including the use of helmets, seat belts, and fall prevention strategies, may also play a role in reducing the incidence of severe brain injuries that can lead to Duret hemorrhages. For families of affected patients, discussions should focus on prognosis, potential complications, and the need for long-term supportive care in cases of survival.
Enhancing Healthcare Team Outcomes
The management of Duret hemorrhages requires a highly coordinated interprofessional approach to optimize patient outcomes due to the severe nature of brainstem injury. Clinicians, particularly neurosurgeons, intensivists, and neurologists, must promptly recognize the signs of increased intracranial pressure and implement strategies to prevent transtentorial herniation, including hyperosmolar therapy, controlled ventilation, and timely surgical decompressive intervention. Advanced clinicians and critical care nurses play a crucial role in continuous neurological monitoring, early detection of clinical deterioration, and ensuring adherence to evidence-based protocols for managing traumatic brain injury. Pharmacists contribute by optimizing medication regimens, including intracranial pressure-lowering agents, anticoagulation reversal strategies, and sedation management to prevent secondary brain insults.
Effective interprofessional communication and care coordination are vital for patients who are critically ill because timely interventions can be lifesaving. Standardized protocols, such as early warning systems and structured handoff tools like SBAR (Situation, Background, Assessment, Recommendation), help ensure that critical information is accurately conveyed among all team members. Physical therapists and rehabilitation specialists also become essential for survivors by aiding in functional recovery and quality-of-life improvement. A patient-centered approach that integrates shared decision-making with family members regarding prognosis, goals of care, and potential long-term care needs enhances patient safety and overall team performance.
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
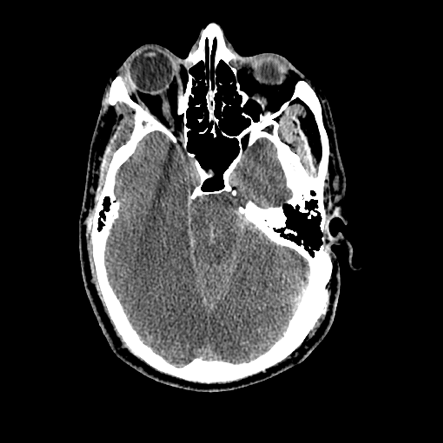
Computed Tomography Scan of a Duret Hemorrhage. A noncontrast head computed tomography (CT) scan reveals a linear hyperdensity in the ventral midbrain and paramedian pontine regions, with obliteration of the perimesencephalic cistern. Additionally, sulcal effacement is observed in the bilateral occipital cortices.
Contributed by B Gogia, MD
References
Parizel PM, Makkat S, Jorens PG, Ozsarlak O, Cras P, Van Goethem JW, van den Hauwe L, Verlooy J, De Schepper AM. Brainstem hemorrhage in descending transtentorial herniation (Duret hemorrhage). Intensive care medicine. 2002 Jan:28(1):85-8 [PubMed PMID: 11819006]
Level 3 (low-level) evidenceWalusinski O, Courrivaud P. Henry Duret (1849-1921): a surgeon and forgotten neurologist. European neurology. 2014:72(3-4):193-202. doi: 10.1159/000361046. Epub 2014 Sep 11 [PubMed PMID: 25227400]
Stiver SI, Gean AD, Manley GT. Survival with good outcome after cerebral herniation and Duret hemorrhage caused by traumatic brain injury. Journal of neurosurgery. 2009 Jun:110(6):1242-6. doi: 10.3171/2008.8.JNS08314. Epub [PubMed PMID: 19012479]
Level 3 (low-level) evidenceEdlow BL, Threlkeld ZD, Fehnel KP, Bodien YG. Recovery of Functional Independence After Traumatic Transtentorial Herniation With Duret Hemorrhages. Frontiers in neurology. 2019:10():1077. doi: 10.3389/fneur.2019.01077. Epub 2019 Oct 9 [PubMed PMID: 31649617]
Quintas S, Palmí Cortés I, Zapata-Wainberg G, López Ruiz R, Vivancos J. Duret haemorrhage during intravenous administration of thrombolytic therapy. Neurologia. 2019 Jun:34(5):340-342. doi: 10.1016/j.nrl.2016.09.006. Epub 2016 Oct 24 [PubMed PMID: 27788939]
Mezaki T. George Gershwin's death and Duret haemorrhage. Lancet (London, England). 2017 Aug 12:390(10095):646. doi: 10.1016/S0140-6736(17)31623-9. Epub [PubMed PMID: 28816130]
Jost GF, Taub E. A fatal epidural hematoma with Duret hemorrhage. The Journal of trauma. 2010 Dec:69(6):1635. doi: 10.1097/TA.0b013e3181de698b. Epub [PubMed PMID: 21150541]
Level 3 (low-level) evidenceBonow RH, Bales JW, Morton RP, Levitt MR, Zhang F. Reversible coma and Duret hemorrhage after intracranial hypotension from remote lumbar spine surgery: case report. Journal of neurosurgery. Spine. 2016 Mar:24(3):389-93. doi: 10.3171/2015.6.SPINE1521. Epub 2015 Nov 20 [PubMed PMID: 26588496]
Level 3 (low-level) evidenceCardinale M, Meaudre E, Cungi PJ, Nguyen C, Esnault P, Joubert C. Duret hemorrhage complicating a sinking skin flap syndrome. British journal of neurosurgery. 2019 Aug:33(4):442-443. doi: 10.1080/02688697.2017.1374350. Epub 2017 Sep 8 [PubMed PMID: 28885045]
Beucler N, Dagain A, Sellier A. Duret Brainstem Hemorrhage Secondary to Large Supratentorial Meningioma. World neurosurgery. 2023 Sep:177():1-2. doi: 10.1016/j.wneu.2023.05.067. Epub 2023 May 24 [PubMed PMID: 37236310]
Nguyen HS, Doan NB, Gelsomino MJ, Shabani S, Mueller WM. Good outcomes in a patient with a Duret hemorrhage from an acute subdural hematoma. International medical case reports journal. 2016:9():15-8. doi: 10.2147/IMCRJ.S95809. Epub 2016 Jan 27 [PubMed PMID: 26869816]
Level 3 (low-level) evidenceBeucler N, Cungi PJ, Dagain A. Duret Brainstem Hemorrhage After Transtentorial Descending Brain Herniation: A Systematic Review and Meta-Analysis. World neurosurgery. 2023 May:173():251-262.e4. doi: 10.1016/j.wneu.2023.02.110. Epub 2023 Mar 2 [PubMed PMID: 36868404]
Level 1 (high-level) evidenceMcKenna C, Fellus J, Barrett AM. False localizing signs in traumatic brain injury. Brain injury. 2009 Jul:23(7):597-601. doi: 10.1080/02699050902973921. Epub [PubMed PMID: 19557561]
Miller NR. Late improvement in upward gaze in a patient with hydrocephalus related Parinaud dorsal midbrain syndrome. The British journal of ophthalmology. 2006 Jan:90(1):123 [PubMed PMID: 16361690]
Level 3 (low-level) evidenceSingla N, Kapoor A, Chatterjee D. Diagnosing early upward cerebellar herniation by computed tomography: A diagnostic boom, a savior. Surgical neurology international. 2016:7():72. doi: 10.4103/2152-7806.185009. Epub 2016 Jun 29 [PubMed PMID: 27453797]
Wang J, Chen L, Liang Y, Chen T, Yuan Y, Yang Y, Fang H, Xie T, Zhuang J. Optimal dose of aerobic exercise for reducing depressive symptoms in children and adolescents: A meta-analysis of randomized controlled trials and dose-response analysis. Journal of affective disorders. 2025 Oct 15:387():119501. doi: 10.1016/j.jad.2025.119501. Epub 2025 May 27 [PubMed PMID: 40441657]
Level 1 (high-level) evidenceBermúdez G, Areitio E. Duret haemorrhage with full recovery. Acta neurochirurgica. 2015 Sep:157(8):1337-8; discussion 1338. doi: 10.1007/s00701-015-2486-5. Epub 2015 Jul 3 [PubMed PMID: 26136197]
Jung Y, Ellenbogen Y, Pirouzmand F. Delayed neurological improvement in a patient with Duret hemorrhage secondary to an acute subdural hematoma: illustrative case. Journal of neurosurgery. Case lessons. 2023 Dec 18:6(25):. pii: CASE23554. doi: 10.3171/CASE23554. Epub 2023 Dec 18 [PubMed PMID: 38109732]
Level 3 (low-level) evidenceGarrido Márquez I, Sánchez Torrente A, Pérez Cuenca E. Duret haemorrhages or brainstem bleeding: An uncommon site of posttraumatic bleeding. Radiologia. 2023 May-Jun:65(3):285-286. doi: 10.1016/j.rxeng.2023.04.001. Epub 2023 May 10 [PubMed PMID: 37268370]
Kamijo Y, Soma K, Kishita R, Hamanaka S. Duret hemorrhage is not always suggestive of poor prognosis: a case of acute severe hyponatremia. The American journal of emergency medicine. 2005 Nov:23(7):908-10 [PubMed PMID: 16291454]
Level 3 (low-level) evidenceFujimoto Y, Aguiar PH, Freitas AB, de Andrade AF, Marino Júnior R. Recovery from Duret hemorrhage: a rare complication after craniotomy--case report. Neurologia medico-chirurgica. 2000 Oct:40(10):508-10 [PubMed PMID: 11098635]
Level 3 (low-level) evidenceBeier AD, Dirks PB. Pediatric brainstem hemorrhages after traumatic brain injury. Journal of neurosurgery. Pediatrics. 2014 Oct:14(4):421-4. doi: 10.3171/2014.7.PEDS13376. Epub 2014 Aug 8 [PubMed PMID: 25105513]
Level 3 (low-level) evidence