Definition/Introduction
The compliance of a system is defined as the change in volume that occurs per unit change in the system's pressure. In simple terms, compliance refers to the ease with which an elastic structure stretches. Therefore, compliance serves as a measurement of a system's elastic resistance.
Pulmonary compliance (C) represents the total compliance of both lungs, measuring the extent to which the lungs expand (change in volume of the lungs) for each unit increase in trans-pulmonary pressure (when sufficient time is allowed for the system to reach equilibrium).[1] Pulmonary compliance is one of the most important concepts underpinning mechanical ventilation to manage respiration in patients in the operating room or intensive care unit (ICU) environment. To better understand pulmonary compliance, specific terminologies require a brief review.
The following formula is useful for calculating compliance:
- Lung compliance (C) = Change in lung volume (V)/Change in transpulmonary pressure (alveolar pressure [Palv] − pleural pressure [Ppl]).
Transpulmonary pressure is the gradient between the intra-alveolar pressure and the pleural pressure outside the lungs, and it primarily measures the force of lung elasticity at each point of respiration (recoil pressure). Alveolar pressure refers to the air pressure within the alveoli, while pleural pressure denotes the pressure of the fluid in the space between the visceral pleura (the layer adhered to the lungs) and the parietal pleura (the lining of the chest wall). Normally, the total compliance of both lungs in an adult is approximately 200 mL/cm H2O. Physicians rely on this concept to understand various pulmonary pathologies, guide therapy, and adjust ventilator pressure and volume settings.
Issues of Concern
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Issues of Concern
Types of Compliance
For practical purposes, lung compliance measurement uses different methods. Based on the measurement method, lung compliance can be categorized as static or dynamic.[2]
Static compliance: This refers to pulmonary compliance measured at a fixed volume with no airflow and fully relaxed muscles. This occurs when the transpulmonary pressure equals the elastic recoil pressure of the lungs, measuring only the elastic resistance. While a simple water manometer was historically used, electrical transducers are now more commonly used for this measurement. In conscious individuals, achieving complete relaxation of the respiratory muscles is challenging. However, the compliance measurement remains valid, as the static pressure difference is unaffected by muscle activity. In paralyzed individuals, such as those in the operating room, static compliance is easily measured using recordings from electrical transducers.
Therapeutically, static compliance is used to determine the optimal level of positive end-expiratory pressure (PEEP), which is calculated using the following formula:
- Cstat = V/(Pplat – PEEP), where
Pplat denotes plateau pressure, and PEEP denotes positive end-expiratory pressure.
Dynamic compliance: This refers to the continuous measurement of pulmonary compliance, calculated at each point to reflect schematic changes during rhythmic breathing.[2] Dynamic compliance monitors both elastic resistance and airway resistance. Airway resistance depends on factors such as air viscosity, density, and the length and radius of the airways. All variables affecting airway resistance, except for the airway radius, remain relatively constant. Therefore, airway resistance can undergo physiological changes based on alterations in the airway's radius.
Compliance Diagram
When lung volume readings are taken at specific pressure points and plotted on a diagram, a pressure-volume curve representing the elastic and airway resistance properties of the lung is obtained (see Image. Comparison of Lung Compliance Curves).[3] The 2 meeting points on this curve are the end-inspiratory and end-expiratory phases; the line connecting these points represents the lung's dynamic compliance. The area between this line and the curves reflects the additional work required to overcome airway resistance during both inspiration and expiration. This curve is also known as the hysteresis curve,[4] which illustrates that the lung is not a perfect elastic structure. More pressure is required to inflate the lungs than to deflate them.
Importance of Compliance
Lung compliance is inversely proportional to elastance, reflecting the elastic resistance of lung tissue (parenchyma) and the surface elastic forces at play. Any changes in these forces can lead to alterations in compliance. Compliance accounts for approximately 65% of the work of breathing. When lung compliance is low, the breathing muscles must exert more effort to inflate the lungs. In certain pathologies, continuous monitoring of the lung compliance curve is essential for understanding the progression of the condition and determining the appropriate therapeutic settings for ventilator management.[5]
Factors Affecting Pulmonary Compliance
Elastic property of the lung tissue: The elastic properties of lung tissue arise from the collagen and elastin fibers interwoven within the lung parenchyma. When the lung is outside the body and in a deflated state, these fibers fully contract due to their elastic nature. As the lung expands, the fibers elongate, generating additional elastic force, similar to a rubber band. Therefore, the flexibility of these fibers is crucial in determining lung compliance. Specific pulmonary pathologies can damage or affect these fibers, impacting overall compliance.
Surface tension elastic force: An important factor affecting lung compliance is the elastic property of the lung, which is influenced by the surface tension of the alveolar lining.[6] The image illustrates the difference in compliance between saline-filled and normal air-filled lungs. Air-filled lungs behave as a distinct elastic structure within the pulmonary system, where flexibility is determined not only by the elastic forces of lung tissue but also by the surface tension exerted by the fluid lining the alveolar walls.[7] When water forms a surface with air, the water molecules exhibit strong, attractive forces toward each other, causing surface contraction—similar to what holds a raindrop together.
Similarly, the water lining the inner surface of the alveoli exerts a force that attempts to expel air and collapse the alveoli. This force is known as surface tension elastic force, with a minimum value of 35 to 41 dyne/cm.[8] As a result, saline-filled lungs have higher compliance than air-filled lungs because the pressure required to expand air-filled lungs is greater than that for saline-filled lungs.
Surfactant: According to Laplace's law, when measuring alveolar pressure using the surface tension exerted by the lining fluid, the formula is:
Pressure = (2×T)/R, where
T is surface tension, and R is the radius of the alveolus.
This indicates that the pressure within smaller alveoli would be higher than that in larger alveoli, potentially leading to the collapse of smaller alveoli. However, in typical scenarios, this collapse does not occur due to the role of surfactants.[8]
A surfactant is a surface-active fluid secreted by type II alveolar epithelial cells lining the alveoli. Surfactants are complex substances composed of the phospholipid dipalmitoylphosphatidylcholine, surfactant proteins, and calcium ions. Surfactants reduce surface tension by partial dissolution. Returning to the mechanics, smaller alveoli have a smaller surface area, resulting in a higher concentration of surfactants and, consequently, lower surface tension.[9] Surfactants have an indirect role in influencing lung compliance by modifying surface tension.
Lung volume: Compliance is related to lung volume, as indicated by the formula connecting volume and pressure. However, specific compliance is calculated using the formula provided below to eliminate this variable.
Specific compliance = Compliance/Functional residual capacity.
Age: This factor has a minimal influence on compliance. Pulmonary compliance tends to increase with age due to structural changes in the elastin fibers of the lungs.[10]
Clinical Significance
Certain pulmonary diseases can lead to changes in lung compliance. The pathologies mentioned below can either increase or decrease lung compliance.
- Emphysema or chronic obstructive pulmonary disease: In both conditions, the lung's elastic recoil is compromised due to genetic factors, such as alpha-1 antitrypsin deficiency, or extrinsic factors like smoking. As a result of reduced elastic recoil, patients exhibit high lung compliance. Their alveolar sacs retain a high residual volume, making it difficult to exhale excess air, which often leads to shortness of breath.
- Pulmonary fibrosis: Environmental pollutants, chemicals, infectious agents, and genetic diseases can lead to fibrosis of the lung tissue. In this condition, lung elastin fibers are replaced by collagen, which is less elastic and reduces lung compliance. As a result, patients must exert more effort to inflate the more rigid lung alveoli.
- Newborn respiratory distress syndrome: Surfactant secretion typically begins between the sixth and seventh months of gestation. Premature newborns may have little or no surfactant in their alveoli at birth, resulting in a significant tendency for their lungs to collapse. As mentioned earlier, surfactant reduces surface tension, thereby increasing lung compliance. The absence of surfactant leads to decreased pulmonary compliance, a condition known as newborn respiratory distress syndrome. This condition can be life-threatening and requires aggressive intervention, including continuous positive pressure breathing.
- Atelectasis or acute respiratory distress syndrome: Atelectasis refers to the collapse of lung alveoli, which usually occurs in the dependent parts of the lungs. Following operative anesthesia, this condition can be a potential complication. In cases of atelectasis, pulmonary compliance decreases due to reduced lung volume, requiring higher pressure to inflate the alveoli. Monitoring techniques such as compliance curves, oximetry, and arterial gas analysis are valuable in the ICU setting.[11]
Media
(Click Image to Enlarge)
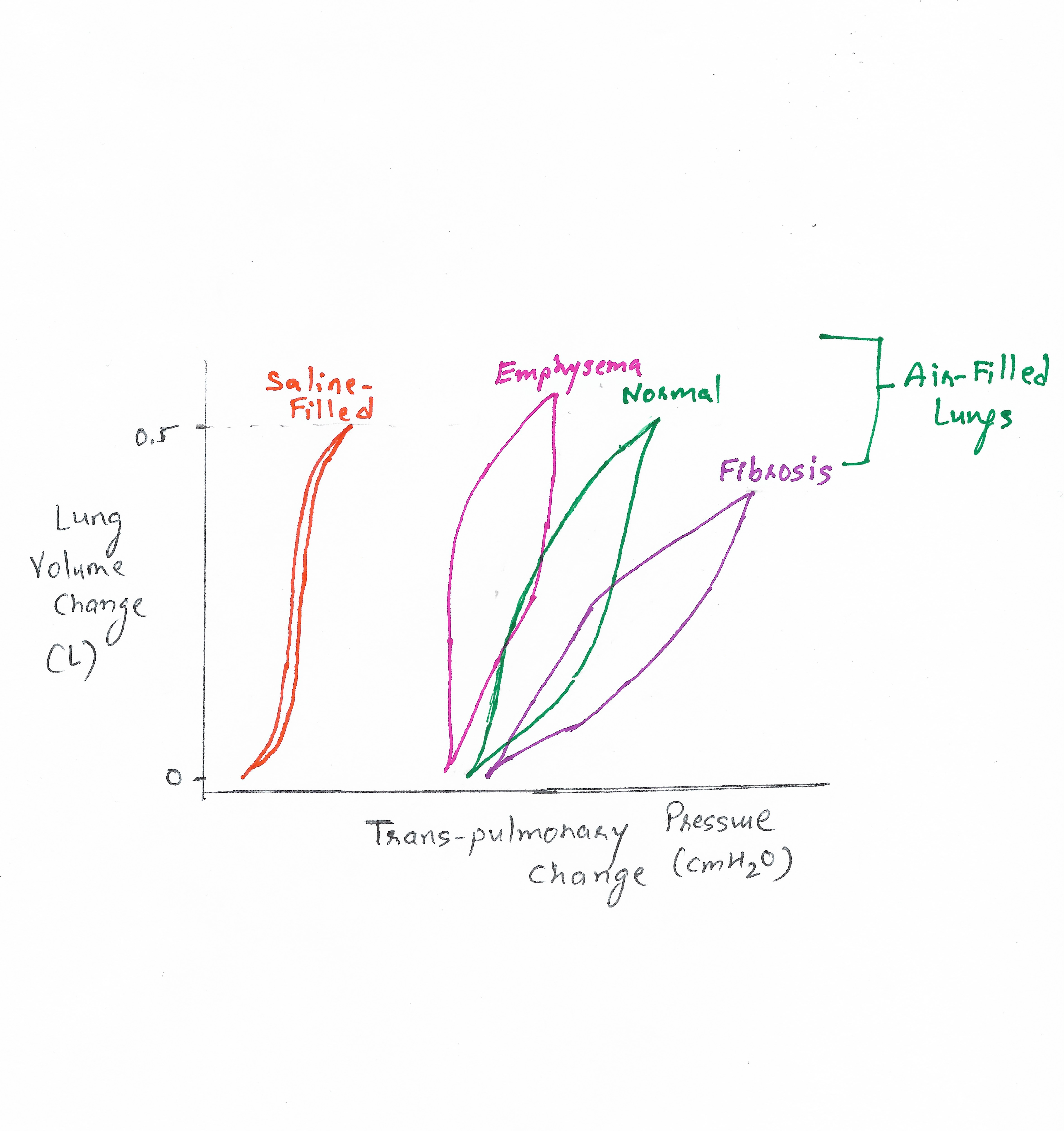
Comparison of Lung Compliance Curves. This diagram compares saline-filled and air-filled lungs and lungs affected by different pathologies, including emphysema and fibrosis. The pressure required to inflate saline-filled lungs is lower than normal air-filled lungs. This difference is primarily attributed to the additional surface tension elastic forces present in air-filled lungs due to the fluid lining the alveolar epithelium.
Contributed by F Moustarah, MD, and J Desai, MBBS
References
MARSHALL R. The physical properties of the lungs in relation to the subdivisions of lung volume. Clinical science. 1957 Aug:16(3):507-15 [PubMed PMID: 13473164]
FRY DL, HYATT RE. Pulmonary mechanics. A unified analysis of the relationship between pressure, volume and gasflow in the lungs of normal and diseased human subjects. The American journal of medicine. 1960 Oct:29():672-89 [PubMed PMID: 13702319]
RAHN H, OTIS AB. The pressure-volume diagram of the thorax and lung. The American journal of physiology. 1946:146(2):161-78 [PubMed PMID: 20982947]
Mercurio MR, Fiascone JM, Lima DM, Jacobs HC. Surface tension and pulmonary compliance in premature rabbits. Journal of applied physiology (Bethesda, Md. : 1985). 1989 May:66(5):2039-44 [PubMed PMID: 2745272]
Level 3 (low-level) evidenceLu Q, Rouby JJ. Measurement of pressure-volume curves in patients on mechanical ventilation: methods and significance. Critical care (London, England). 2000:4(2):91-100 [PubMed PMID: 11094498]
Sera T, Fujioka H, Yokota H, Makinouchi A, Himeno R, Schroter RC, Tanishita K. Localized compliance of small airways in excised rat lungs using microfocal X-ray computed tomography. Journal of applied physiology (Bethesda, Md. : 1985). 2004 May:96(5):1665-73 [PubMed PMID: 14766787]
Level 3 (low-level) evidenceWest JB. History of respiratory mechanics prior to World War II. Comprehensive Physiology. 2012 Jan:2(1):609-19. doi: 10.1002/cphy.c080112. Epub [PubMed PMID: 23728981]
Morgan TE. Pulmonary surfactant. The New England journal of medicine. 1971 May 27:284(21):1185-93 [PubMed PMID: 4929384]
Level 3 (low-level) evidenceBROWN ES, JOHNSON RP, CLEMENTS JA. Pulmonary surface tension. Journal of applied physiology. 1959 Sep:14():717-20 [PubMed PMID: 13804921]
Lalley PM. The aging respiratory system--pulmonary structure, function and neural control. Respiratory physiology & neurobiology. 2013 Jul 1:187(3):199-210. doi: 10.1016/j.resp.2013.03.012. Epub 2013 Apr 6 [PubMed PMID: 23570957]
Duggan M, Kavanagh BP. Pulmonary atelectasis: a pathogenic perioperative entity. Anesthesiology. 2005 Apr:102(4):838-54 [PubMed PMID: 15791115]