Introduction
Tattoos have been applied to human skin since prehistory as rights of passage, indications of group membership, aesthetic enhancements, sequelae of trauma, components of medical procedures, and even as penalties. Presumably, the desire to remove them has existed for just as long. Early tattoo removal methods included cryotherapy, surgical excision, and skin resurfacing techniques, such as dermabrasion or chemical peeling. Cryotherapy and resection of the tattooed skin tend to leave residual textural changes or surgical scars and may not be feasible for large tattoos. On the other hand, skin resurfacing only reaches down to the papillary dermis, which may be effective for removing amateur tattoos but is unlikely to affect deeper, professional tattoos.
The first device that produced light amplificated by the stimulated emission of radiation (laser) was built at Hughes Research Laboratories in 1960 and used a synthetic ruby as a lasing medium; the first report of a laser used for tattoo removal followed in 1965, using ruby as the lasing medium as well.[1] The advantage of lasers over other modalities of tattoo removal is that lasers can target the pigment in tattoos specifically and thereby minimize damage to the surrounding skin, thus lowering the risk of scarring and dyspigmentation while preserving or enhancing efficacy. Because laser light is, by definition, collimated, coherent, and monochromatic, each wavelength of light produced by a laser will be absorbed primarily by specific target chromophore molecules, resulting in selective photothermolysis.[2][3]
The keys to successful tattoo removal, therefore, are the selection of the appropriate laser wavelength in the context of the color of the tattoo and the surrounding skin and ensuring that the energy pulses are delivered in such a way as to minimize thermal injury to the surrounding tissue. Early lasers delivered energy pulses with durations in the millisecond range, which had the effect of overheating and damaging the tissue surrounding the chromophore, leading to more inflammation, scarring, and injury to melanocytes that caused subsequent hypo- or hyperpigmentation.[4] These adverse events are more likely to occur when the pulse duration exceeds the thermal relaxation time of the tissue—the time it takes for the tissue to lose 50% of the heat it gains from the laser pulse.
This time may be as brief as 10 ns for tattoo particles, necessitating a very short laser pulse to avoid exceeding the thermal relaxation time. The solution came from so-called quality-switched (QS or Q-switched) lasers, which produce pulse widths in the nanosecond range. These lasers have become a mainstay of tattoo removal because of their ability to remove or lighten pigments of multiple colors while decreasing the incidence of post-treatment burns, scars, and hypo- or hyperpigmentation. Further technological advancements have more recently resulted in the development of picosecond lasers, which can deliver energy in such short pulses that laser beam emission begins and ends before the first photons reach the skin.[5][6]
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Tattoos may occur for various reasons, including traumatic implantation of debris within the skin, a blast injury, iatrogenic pigment impregnation into soft tissue, and dental amalgam tattooing. However, the most common source of a tattoo is elective placement with a needle or tattoo gun.[7] Determining the etiology of the tattoo in question, as the mechanism of pigment implantation, will provide a clue regarding its histological depth and inform the plan for removing it, which is essential. Traumatic tattoos caused by explosions, such as with fireworks or gunpowder, can result in combustible material being embedded in the skin; great care should be taken in these circumstances since the application of the laser can ignite these particles and result in small explosions that endanger the patient and the laser operator.
While not as potentially dangerous as traumatic tattoos, elective tattoos may also provide surprises for the patient and the laser operator; many inks used in tattooing are combinations of multiple pigments, some more responsive to laser treatments than others. In these cases, treating the tattoo may cause it to change colors or only lighten slightly rather than fading to a noticeable extent. Some inks contain ferric oxide or titanium dioxide, which may undergo chemical reduction if heated by a laser, thus paradoxically darkening a treated tattoo.[8]
Epidemiology
Over the years, tattoos have become increasingly popular. According to a 2016 Harris Poll, 3 in 10 adults in the United States have at least 1 tattoo, compared to 2 in 10 adults in 2012, and a 2023 Pew Research survey (Pew survey) saw a further increase to 32%, with 22% of Americans having more than 1 tattoo. The Pew study reported that 38% of women and 27% of men in the United States have tattoos, with over half of women in the 18 to 49 age group having at least 1. In general, younger people are more likely to have tattoos, with over 40% of Americans in the 18 to 49 age group reporting 1 or more tattoos, but only 13% in those aged 65 and older.
Tattoos are most common in the Black population, with a 39% prevalence, and least common among those in the Asian population, with a 14% prevalence. Hispanic and White individuals are in the middle, with prevalences of 35% and 32%, respectively. There appear to be other demographic correlations with tattoos; 24% of college graduates and 21% of those with a graduate degree have tattoos, but 37% of individuals who did not complete college have tattoos. Tattooing is more common among lower-income adults (43%) and less common among high earners (21%). Tattoos are more common in individuals who do not consider themselves religious (41%) than those who do (29%). Lastly, 31% of heterosexual individuals in the United States have at least one tattoo, while 51% of gay, lesbian, and bisexual Americans do, with 68% of homosexual women reporting tattoos.
Individuals who smoke cigarettes are twice as likely to have tattoos than people who do not, and people who have reported having a history of alcohol or drug abuse are also twice as likely to have tattoos as those without such a history. On the other hand, there are no discernable relationships between liberal and conservative political views, urban versus suburban or rural living, and having served in the armed services or not with the presence of tattoos. Perhaps most importantly, 24% of individuals with tattoos regret the decision. Rates of regret are highest in Hispanic individuals (30%) and those without a college degree (25%). Eleven percent of individuals with tattoos have had or plan to undergo tattoo removal. Over 52,000 tattoo removal procedures were performed in the United States in 2018 alone.
Pathophysiology
Amateur tattoos are more superficially in the papillary dermis, whereas professional tattoos are located deeper in the reticular dermis. This fact often makes the removal of amateur tattoos easier than professional tattoos. Professional tattoos are also likely to be more elaborate, with multiple different pigments that may complicate removal by laser. While immune system action on tattoo particles begins the moment the pigment is placed into the skin, the comparatively large size of the ink particles, up to 970 nm, makes processing by white blood cells very challenging.[9]
Laser tattoo removal breaks down the pigment particles through photothermal (heat) and photomechanical (shockwave due to thermal expansion) effects. The resulting smaller particles can then be eliminated via phagocytosis by macrophages.[10] In some cases, however, macrophages may initiate an immune response that leads to a hypersensitivity reaction manifesting as erythema, edema, pruritus, urticaria, or even anaphylaxis.[11]
History and Physical
A thorough history is important to gather information about the tattoo to be treated and the patient receiving the treatment. Important points regarding the tattoo include its age and whether it is a "cover-up" layer or a "double" tattoo. Older tattoos have already undergone some degradation due to ultraviolet light exposure and may require fewer treatments to remove. Double tattoos, on the other hand, have more pigment deposited in the dermis, which means that an unexpectedly large proportion of the energy may be absorbed by the laser's chromophore, potentially resulting in burns and scarring. Tattoos that have been treated previously but have changed color or darkened may require more treatments than might otherwise be expected and may not be able to be removed completely.
Concerning the patient's medical history, it is important to know whether or not the patient has had prior tattoo removal and, if so, whether there were any complications. Additionally, any history of wound-healing difficulties, hypertrophic scarring, or keloids should be elicited. If there is a history of herpes simplex outbreaks, particularly in the context of facial tattoo removal, prophylactic antiviral medications should be provided.[12] Lastly, a medication history should be taken.[13][14]
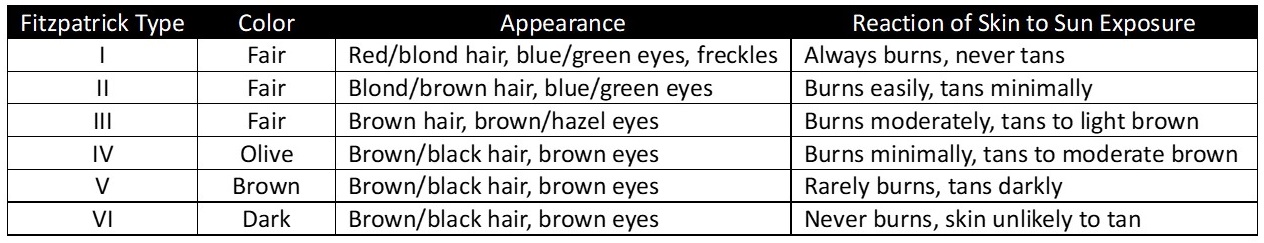
The physical examination should note each of the different colors of the tattoo, as more intricate and colorful tattoos—particularly those with orange, yellow, and white pigments (often found in pink and light blue inks)—are more difficult to remove. Identifying the colors that are present will inform the selection of the appropriate laser. Determining the age of the tattoo and how faded it is will also provide some prognostic information about the number of treatments likely to be required for removal. Most important, however, is noting the patient's skin color. Typically recorded using the Fitzpatrick scale, the amount of pigmentation in the patient's skin will determine the risk of post-treatment dyspigmentation and, therefore, which laser is likely to be safest (see Table. Fitzpatrick Skin Types, Table) as darker skin is more prone to hypo- or hyperpigmentation after exposure to laser energy.[15]
Evaluation
Patients should be counseled that tattoo removal takes anywhere from 4 to 15 treatments depending on the age, color, quality, and mechanism of tattoo placement. Also, discuss the importance of sun avoidance pre- and post-treatment due to the risk of dyspigmentation. Photographs and written informed consent should be obtained initially, before every session, and after the treatment. The risks of the procedure should be discussed, which can include the following:
- Pain
- Bleeding
- Infection
- Loss of or damage to vision
- Damage to surrounding anatomy
- Need for additional procedures
- Hyperpigmentation
- Hypopigmentation
- Burning
- Blistering
- Scarring
- Skin texture change
- Unpredictable treatment response
- Color change within the tattoo, including paradoxical darkening
- Dissatisfaction with the outcome
While it is only an estimate, the Kirby Desai scale provides a means of estimating the number of treatments that will be required to clear the tattoo. The scale assigns points for the tattoo's location, with the head and neck being optimal and the distal extremity more challenging, the coloration, with black ink only being preferable to multicolored tattoos, the amount of ink, with superficial, amateur tattoos most favorable, and the amount of scarring and ink layering present, with less being better in both categories.[16]
Treatment / Management
The patient’s skin should be prepped with alcohol or chlorhexidine. Due to the fire risk, alcohol should be completely dry before beginning the procedure. Because laser treatments tend to be painful, the area in question may be anesthetized preoperatively with topical anesthetic cream (2.5% lidocaine-2.5% prilocaine or similar) or injection with a local anesthetic agent (2% lidocaine, 1% bupivacaine or similar) to produce either a regional block or anesthesia of the tattoo itself. If a topical anesthetic is used, it should be placed under an occlusive dressing for 45 to 60 minutes and then completely removed before starting treatment.
Before using the laser, it is critical to follow certain precautions. Everyone must wear safety glasses or goggles rated for the laser wavelength during treatment. Depending on where the tattoo is located, the patient may wear an identical pair of glasses or goggles to those the healthcare team members are using, or if the tattoo is near the eyes, metal eye shields or corneal protectors may be more practical. If there are windows in the treatment room, they should be shuttered to prevent the laser light from escaping and causing an injury via direct eye exposure or reflection of the laser light. The laser most dangerous to the human eye is the neodymium-doped yttrium-aluminum-garnet (Nd:YAG) laser because its long wavelength and affinity for melanin make it capable of reaching through the eye, all the way back to the melanocytes within the retina. Ideally, laser-safe masks should be worn by the healthcare team members to prevent inhalation of aerosolized epithelial particles as well.
For the first session, a "test patch" may be performed. This involves firing the laser at a single, small spot on the tattoo to determine how it responds to treatment at specific settings; test patches are most commonly employed when the patient has dark skin, a history of exuberant scarring, or if there is a concern that treating the tattoo with the laser will result in paradoxical color change.[17] A full treatment may be scheduled if the test patch does not exhibit any undesirable developments after 2 to 4 weeks.
The machines used for laser tattoo removal typically default to recommended settings for starting treatment, and these settings can generally be used very safely, if not always very effectively, due to their conservative fluences. Fluence is the energy density deposited by the laser into the tissue in 1 pulse, measured in J/cm2. The fluence must be frequently increased above the default setting to produce a clinically significant effect. As the tattoo lightens with subsequent treatments, the fluence may need to be increased because of the lower availability of chromophores to absorb the laser energy. For QS lasers, such as the ruby and Nd:YAG lasers, fluences of 4 to 8 J/cm2 and 6 to 12 J/cm2 may be appropriate, but picosecond lasers will typically require lower fluence levels to achieve the same effect, such as 1 to 2 J/cm2 for the picosecond alexandrite laser.[18][19]
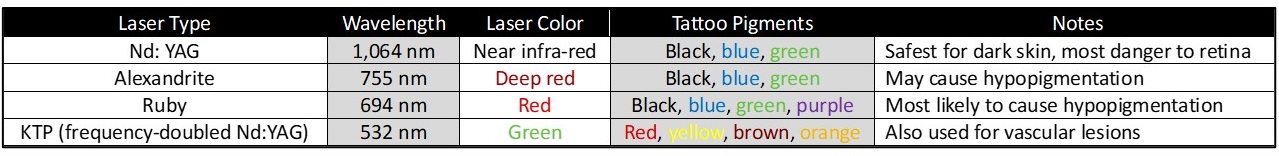
With ruby, alexandrite, Nd:YAG, and frequency-doubled Nd:YAG (also known as potassium-titanyl-phosphate [KTP] because of the additional crystal used) lasers available for tattoo removal, selecting the most appropriate one for an individual patient's tattoo colors and skin pigmentation may be challenging. The alexandrite and ruby lasers emit deep, red-colored beams (755 nm and 694 nm, respectively), while the KTP laser is green (532 nm), and the Nd:YAG laser operates in the near infra-red range (1064 nm). As a general rule, tattoos are not treated effectively with lasers that produce light of the same color as the ink because that is the color reflected most efficiently by the pigment; for example, a ruby laser is liable to have little impact on a red tattoo, but treatment with a KTP laser would likely be successful. The ruby laser is best for blue, green, and purple pigments, the alexandrite for blue and green, the Nd:YAG for blue and green, and the KTP laser for red, yellow, brown, and orange. Because black pigment absorbs a broad spectrum of light wavelengths, the ruby, alexandrite, and 1064 nm Nd:YAG lasers can be effective for removing black tattoos, or even for tattoos that have undergone paradoxical darkening, although these tattoos may not clear completely even with a great many treatments (see Table. Type of Lasers for Tattoo Removal, Table).[20][21][22]
When firing the laser, the spots should overlap by 10% to 20%, and the most practical spot size for the tattoo being treated should be used. Larger spot sizes not only permit faster treatment of the tattoo but also reduce the relative amount of energy lost to diffraction within the skin, which occurs predominantly around the perimeter of the spot, hence the need for overlapping.[23][24] Cooling with cold air blown across the tattoo or periodic application of cold packs to the treated area will reduce patient discomfort and swelling.
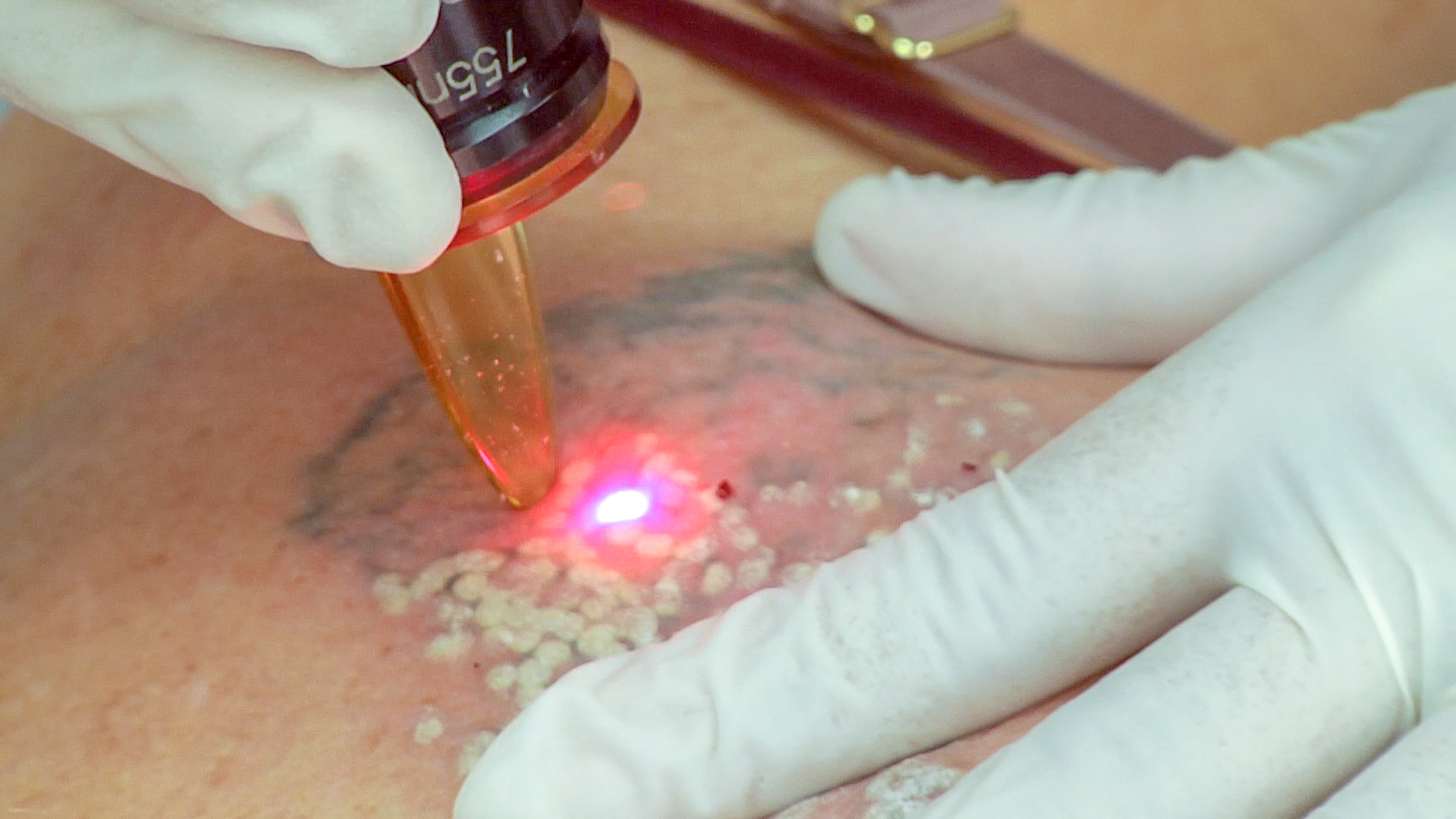
Appropriate settings on the laser will result in immediate "frosting" of the tattoo during treatment, which represents the formation of gas bubbles in the skin; the lowest fluence that produces this reaction should be used to reduce thermal injury to the skin (see Image. Q-switched Alexandrite Laser). The white discoloration will typically clear within 20 minutes, permitting observation of any color change within the tattoo. Titrating laser settings to this clinical endpoint, as the extent of tattoo pigment reduction is not clinically apparent initially, and additional lightening will occur over the ensuing weeks as the degraded pigment particles are phagocytosed and cleared, is essential. If pinpoint bleeding or tissue spatter occurs, the fluence should be lowered immediately, as these are signs of excessive energy delivery.
Typically, laser sessions are repeated every 6 to 8 weeks, as tolerated, until the tattoo is completely cleared, no further progress is being made, or the patient elects to discontinue treatment. To expedite tattoo clearance, however, some protocols permit multiple treatment passes to be made in the same session. In 2012, Kossida et al developed the "R20" method, which involves repeating the treatment up to 4 times at 20-minute intervals, thereby allowing the frosting to clear between passes.[25] The "R0" method, described the following year by Reddy et al, permits multiple passes without waiting periods between them via the use of topical perfluorodecalin to clear the gas bubbles in the tissue twice as rapidly as when they are allowed to clear spontaneously (see Image. R0 Protocol With Q-switched Nd:YAG Laser).[26]
In contrast to the ruby, alexandrite, KTP, and Nd:YAG lasers, which are considered non-ablative, some authors advocate the use of fractionated ablative lasers, such as carbon dioxide and erbium-doped yttrium-aluminum-garnet (Er:YAG) lasers, to remove superficial pigment, like traumatic and amateur tattoos, either alone or in combination with non-ablative lasers.[27][28] Ablative lasers vaporize the epidermis and superficial dermis by targeting water as their chromophore, thereby permitting the pigment particles to be cleared during the healing process. Ablative lasers have also shown promise for treating refractory tattoos, such as those with light-colored ink or those that have undergone paradoxical darkening.[29] These lasers are typically avoided for treating patients with dark skin, however, particularly if energy is delivered with a continuous wave rather than via a fractionated system.(B3)
Differential Diagnosis
Numerous lasers are available to remove different colors of tattoo ink, but other nonselective tattoo removal methods are also available. Ablative options, such as carbon dioxide and Er:YAG lasers, can be used for superficial or recalcitrant tattoos. Dermabrasion, either manual or with powered instrumentation, may be used similarly to ablative lasers. At the same time, liquid nitrogen and chemical peeling agents, such as trichloroacetic acid, are less precisely applied and are therefore less commonly employed. Tattoos may also be excised surgically, although doing so exchanges a tattoo for a scar, and excising large sections of skin to remove more extensive tattoos is often not feasible.
Prognosis
The efficacy of laser tattoo removal depends on several factors—most importantly, the color of the ink, the color of the patient's skin, and the wavelength and pulse duration of the laser being used. Carbon-based black tattoos in fair-skinned individuals treated with QS ruby, QS alexandrite, or QS Nd:YAG lasers have more than a 90% chance of clearance and a low incidence of complications.[30] For darker-skinned patients, the QS Nd:YAG laser is the modality of choice, although the QS alexandrite laser is also safe and effective.[31][32]
The ruby laser, on the other hand, poses a higher risk of hypopigmentation in these patients.[33] Newer technologies, such as picosecond lasers, are likely even safer for darker-skinned patients (Fitzpatrick type IV-VI) and seem to be both more effective and more comfortable than QS lasers for pain during and after treatment (see Image. Picosecond Alexandrite Tattoo Removal Results).[34][35][36] Overall, rates of complete tattoo clearance are in the 50% range (see Image. Tattoo Removal, Before and After).[31][35]
Complications
The most likely complication of laser tattoo removal is a requirement for more treatments than originally anticipated or unsatisfactory clearing of the tattoo, which may include residual pigment, a change in color or darkening, or a persistent outline of the artwork. Long-term or permanent skin changes may also occur, including alterations in texture and color. Hyperpigmentation is more common than hypopigmentation, although hypopigmentation is more likely to be permanent. Hyperpigmentation is treated with topical bleaching agents, such as 4% hydroquinone cream, while hypopigmentation may be treated with steroids to reduce the causative inflammation or with exposure to blue or ultraviolet light to stimulate melanin production.[37] Poor wound healing, such as blistering, infection, and scarring may occur, as can infection, although this is not common. If the settings employed are too aggressive, burning, skin sloughing, and scarring may result.
Postoperative and Rehabilitation Care
Edema, erythema, and pruritus commonly develop within the first 24 hours after treatment, and they typically subside within 1 to 2 weeks. There may also be crusting or blistering, which should be cleaned to reduce the risk of infection; large blisters may be drained if uncomfortable, but smaller ones tend to resolve spontaneously within a few days. Some clinicians recommend using emollients or antibiotic ointments, but this is not universally practiced. Picking at crusts may increase the risk of infection, and patients are advised to avoid this. Likewise, strenuous exercise and excessive heat (hot showers or saunas) must be avoided for 24 to 48 hours. Sun exposure should be minimized to the greatest extent for at least 2 weeks after treatment to minimize pigmentary changes. If sun exposure cannot be avoided, a topical sun protection agent with a solar protection factor of at least 30 should be applied.
Deterrence and Patient Education
Tattoo regret appears to be quite common in individuals who obtained their tattoos as teenagers, but other factors are also strongly associated with tattoo regret. Being intoxicated with alcohol or recreational drugs at the time of tattoo placement and obtaining a tattoo under peer pressure makes people 3 times more likely to regret the tattoo compared to placement with unimpaired cognition and a lack of external influence. Placement in obvious areas such as the head, neck, hand, or fingers makes individuals with tattoos approximately twice as likely to regret their tattoos as placement in other locations. Avoiding these situations may reduce the risk of tattoo regret and lower the chance of pursuing laser removal.[38]
If tattoo removal is being considered, seeking a board-certified dermatologist or plastic surgeon to perform or supervise the procedure is recommended to decrease the risk of complications. Depending on regional laser-use regulations, nurses staff numerous tattoo removal clinics, nonphysician healthcare providers, tattoo artists, and other nonmedical professionals. For example, in New Jersey and Ohio, only physicians can use a medical laser, but most other states allow nonphysicians to remove tattoos. Many nonphysicians are highly competent and experienced; however, it is important for patients to exercise due diligence in ensuring they seek care at reputable institutions. Patients with dark skin, extensive tattoos, or multicolored tattoos should be the most careful when selecting laser tattoo removal providers, as they have the highest a priori risk of suboptimal outcomes.
Enhancing Healthcare Team Outcomes
Nonphysician healthcare professionals such as nurse practitioners, physician associates, registered nurses, and technicians often remove tattoos using laser energy. For this reason, laser operators must have appropriate training and supervision, if necessary. Not only should laser operators be able to communicate the risks, benefits, and alternatives of laser tattoo removal to patients to set reasonable expectations before beginning treatment, but operators should be able to select optimal laser settings based on patient skin color, tattoo color(s), and patient goals. Furthermore, every laser operator should be an expert in laser safety, ensuring that the risks of fire and eye injury to the patient and healthcare team members are minimized to the greatest extent possible.[39][40]
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
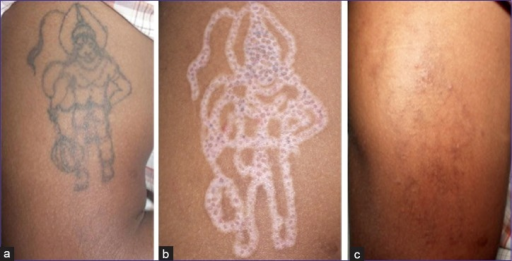
R0 Protocol With Q-switched Nd:YAG Laser. The images show the results of 4 passes in a single session. A) Preoperative appearance of tattoo. B) One week after treatment. C) One month after treatment.
Shah SD, Aurangabadkar SJ. Newer trends in laser tattoo removal. J Cutan Aesthet Surg. 2015;8(1):25-29.
(Click Image to Enlarge)
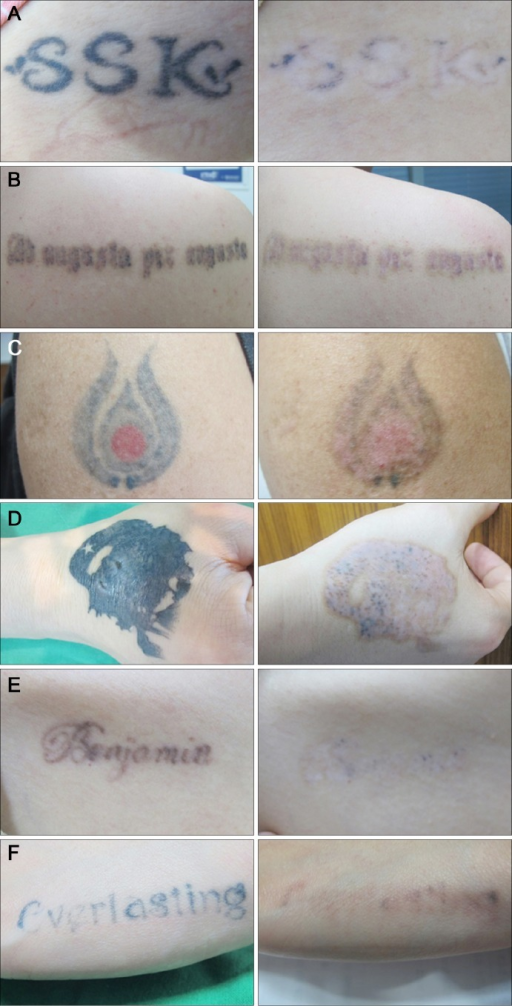
Picosecond Alexandrite Tattoo Removal Results. The images show results after laser treatment in various tattoos; note that most of the tattoos look substantially lighter, but all have some residual ink at the conclusion of treatment.
Lee SH, Lee MH, Noh TK, et al. Successful treatment of tattoos with a picosecond 755-nm alexandrite laser in Asian skin. Ann Dermatol. 2016;28(5):673–675.
References
GOLDMAN L, WILSON RG, HORNBY P, MEYER RG. RADIATION FROM A Q-SWITCHED RUBY LASER. EFFECT OF REPEATED IMPACTS OF POWER OUTPUT OF 10 MEGAWATTS ON A TATTOO OF MAN. The Journal of investigative dermatology. 1965 Jan:44():69-71 [PubMed PMID: 14264287]
Anderson RR, Parrish JA. Selective photothermolysis: precise microsurgery by selective absorption of pulsed radiation. Science (New York, N.Y.). 1983 Apr 29:220(4596):524-7 [PubMed PMID: 6836297]
Level 3 (low-level) evidenceBäumler W, Weiß KT. Laser assisted tattoo removal - state of the art and new developments. Photochemical & photobiological sciences : Official journal of the European Photochemistry Association and the European Society for Photobiology. 2019 Feb 13:18(2):349-358. doi: 10.1039/c8pp00416a. Epub [PubMed PMID: 30452057]
Prohaska J, Hohman MH. Laser Complications. StatPearls. 2025 Jan:(): [PubMed PMID: 30335281]
Kung KY, Shek SY, Yeung CK, Chan HH. Evaluation of the safety and efficacy of the dual wavelength picosecond laser for the treatment of benign pigmented lesions in Asians. Lasers in surgery and medicine. 2019 Jan:51(1):14-22. doi: 10.1002/lsm.23028. Epub 2018 Oct 25 [PubMed PMID: 30357871]
Vangipuram R, Hamill SS, Friedman PM. Accelerated tattoo removal with acoustic shock wave therapy in conjunction with a picosecond laser. Lasers in surgery and medicine. 2018 Sep:50(9):890-892. doi: 10.1002/lsm.22945. Epub 2018 Jun 25 [PubMed PMID: 29938802]
Jeon H, Geronemus RG. Successful treatment of a traumatic tattoo in a pediatric patient using a 755-nm picosecond laser. Pediatric dermatology. 2018 Nov:35(6):e430-e431. doi: 10.1111/pde.13668. Epub 2018 Oct 10 [PubMed PMID: 30303558]
Bernstein EF. Laser tattoo removal. Seminars in plastic surgery. 2007 Aug:21(3):175-92. doi: 10.1055/s-2007-991186. Epub [PubMed PMID: 20567669]
Grant CA, Twigg PC, Baker R, Tobin DJ. Tattoo ink nanoparticles in skin tissue and fibroblasts. Beilstein journal of nanotechnology. 2015:6():1183-91. doi: 10.3762/bjnano.6.120. Epub 2015 May 20 [PubMed PMID: 26171294]
Murphy MJ. High speed ink aggregates are ejected from tattoos during Q-switched Nd:YAG laser treatments. Lasers in surgery and medicine. 2018 Mar 25:():. doi: 10.1002/lsm.22817. Epub 2018 Mar 25 [PubMed PMID: 29575066]
Tjipta A, Ramadhan H, Lubis RA. Immune Response in Laser Tattoo Removal: A Systematic Review. Journal of lasers in medical sciences. 2023:14():e66. doi: 10.34172/jlms.2023.66. Epub 2023 Dec 27 [PubMed PMID: 38318216]
Level 1 (high-level) evidenceGilbert S, McBurney E. Use of valacyclovir for herpes simplex virus-1 (HSV-1) prophylaxis after facial resurfacing: A randomized clinical trial of dosing regimens. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2000 Jan:26(1):50-4 [PubMed PMID: 10632686]
Level 1 (high-level) evidenceSpring LK, Krakowski AC, Alam M, Bhatia A, Brauer J, Cohen J, Del Rosso JQ, Diaz L, Dover J, Eichenfield LF, Gurtner GC, Hanke CW, Jahnke MN, Kelly KM, Khetarpal S, Kinney MA, Levy ML, Leyden J, Longaker MT, Munavalli GS, Ozog DM, Prather H, Shumaker PR, Tanzi E, Torres A, Velez MW, Waldman AB, Yan AC, Zaenglein AL. Isotretinoin and Timing of Procedural Interventions: A Systematic Review With Consensus Recommendations. JAMA dermatology. 2017 Aug 1:153(8):802-809. doi: 10.1001/jamadermatol.2017.2077. Epub [PubMed PMID: 28658462]
Level 1 (high-level) evidenceCohen PR, Ross EV. Q-Switched Alexandrite Laser-induced Chrysiasis. The Journal of clinical and aesthetic dermatology. 2015 Sep:8(9):48-53 [PubMed PMID: 26430491]
Klein A, Rittmann I, Hiller KA, Landthaler M, Bäumler W. An Internet-based survey on characteristics of laser tattoo removal and associated side effects. Lasers in medical science. 2014 Mar:29(2):729-38. doi: 10.1007/s10103-013-1395-1. Epub 2013 Aug 2 [PubMed PMID: 23907603]
Level 3 (low-level) evidenceKirby W, Desai A, Desai T, Kartono F, Geeta P. The Kirby-Desai Scale: A Proposed Scale to Assess Tattoo-removal Treatments. The Journal of clinical and aesthetic dermatology. 2009 Mar:2(3):32-7 [PubMed PMID: 20729941]
Ortiz AE, Alster TS. Rising concern over cosmetic tattoos. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2012 Mar:38(3):424-9. doi: 10.1111/j.1524-4725.2011.02202.x. Epub 2011 Nov 2 [PubMed PMID: 22093105]
Taylor CR, Gange RW, Dover JS, Flotte TJ, Gonzalez E, Michaud N, Anderson RR. Treatment of tattoos by Q-switched ruby laser. A dose-response study. Archives of dermatology. 1990 Jul:126(7):893-9 [PubMed PMID: 2360836]
Kilmer SL, Lee MS, Grevelink JM, Flotte TJ, Anderson RR. The Q-switched Nd:YAG laser effectively treats tattoos. A controlled, dose-response study. Archives of dermatology. 1993 Aug:129(8):971-8 [PubMed PMID: 8352621]
Zelickson BD, Mehregan DA, Zarrin AA, Coles C, Hartwig P, Olson S, Leaf-Davis J. Clinical, histologic, and ultrastructural evaluation of tattoos treated with three laser systems. Lasers in surgery and medicine. 1994:15(4):364-72 [PubMed PMID: 7885170]
Anderson RR, Geronemus R, Kilmer SL, Farinelli W, Fitzpatrick RE. Cosmetic tattoo ink darkening. A complication of Q-switched and pulsed-laser treatment. Archives of dermatology. 1993 Aug:129(8):1010-4 [PubMed PMID: 8352605]
Fitzpatrick RE, Lupton JR. Successful treatment of treatment-resistant laser-induced pigment darkening of a cosmetic tattoo. Lasers in surgery and medicine. 2000:27(4):358-61 [PubMed PMID: 11074513]
Karsai S, Pfirrmann G, Hammes S, Raulin C. Treatment of resistant tattoos using a new generation Q-switched Nd:YAG laser: influence of beam profile and spot size on clearance success. Lasers in surgery and medicine. 2008 Feb:40(2):139-45. doi: 10.1002/lsm.20605. Epub [PubMed PMID: 18306154]
Bernstein EF, Kornbluth S, Brown DB, Black J. Treatment of spider veins using a 10 millisecond pulse-duration frequency-doubled neodymium YAG laser. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 1999 Apr:25(4):316-20 [PubMed PMID: 10417590]
Kossida T, Rigopoulos D, Katsambas A, Anderson RR. Optimal tattoo removal in a single laser session based on the method of repeated exposures. Journal of the American Academy of Dermatology. 2012 Feb:66(2):271-7. doi: 10.1016/j.jaad.2011.07.024. Epub 2011 Oct 27 [PubMed PMID: 22036610]
Reddy KK, Brauer JA, Anolik R, Bernstein L, Brightman L, Hale E, Karen J, Weiss E, Geronemus RG. Topical perfluorodecalin resolves immediate whitening reactions and allows rapid effective multiple pass treatment of tattoos. Lasers in surgery and medicine. 2013 Feb:45(2):76-80. doi: 10.1002/lsm.22106. Epub 2012 Dec 19 [PubMed PMID: 23255145]
Seitz AT, Grunewald S, Wagner JA, Simon JC, Paasch U. Fractional CO2 laser is as effective as Q-switched ruby laser for the initial treatment of a traumatic tattoo. Journal of cosmetic and laser therapy : official publication of the European Society for Laser Dermatology. 2014 Dec:16(6):303-5. doi: 10.3109/14764172.2014.956669. Epub 2014 Sep 25 [PubMed PMID: 25148407]
Weiss ET, Geronemus RG. Combining fractional resurfacing and Q-switched ruby laser for tattoo removal. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2011 Jan:37(1):97-9. doi: 10.1111/j.1524-4725.2010.01821.x. Epub 2010 Nov 12 [PubMed PMID: 21073602]
Wang CC, Huang CL, Yang AH, Chen CK, Lee SC, Leu FJ. Comparison of two Q-switched lasers and a short-pulse erbium-doped yttrium aluminum garnet laser for treatment of cosmetic tattoos containing titanium and iron in an animal model. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 2010 Nov:36(11):1656-63. doi: 10.1111/j.1524-4725.2010.01714.x. Epub 2010 Sep 14 [PubMed PMID: 20840495]
Level 3 (low-level) evidenceLapidoth M, Aharonowitz G. Tattoo removal among Ethiopian Jews in Israel: tradition faces technology. Journal of the American Academy of Dermatology. 2004 Dec:51(6):906-9 [PubMed PMID: 15583581]
Jones A, Roddey P, Orengo I, Rosen T. The Q-switched ND:YAG laser effectively treats tattoos in darkly pigmented skin. Dermatologic surgery : official publication for American Society for Dermatologic Surgery [et al.]. 1996 Dec:22(12):999-1001 [PubMed PMID: 9078310]
Bukhari IA. Removal of amateur blue-black tattoos in Arabic women of skin type (III-IV) with Q-switched alexandrite laser. Journal of cosmetic dermatology. 2005 Jun:4(2):107-10 [PubMed PMID: 17166208]
Ho SG, Goh CL. Laser tattoo removal: a clinical update. Journal of cutaneous and aesthetic surgery. 2015 Jan-Mar:8(1):9-15. doi: 10.4103/0974-2077.155066. Epub [PubMed PMID: 25949017]
Haimovic A, Brauer JA, Cindy Bae YS, Geronemus RG. Safety of a picosecond laser with diffractive lens array (DLA) in the treatment of Fitzpatrick skin types IV to VI: A retrospective review. Journal of the American Academy of Dermatology. 2016 May:74(5):931-6. doi: 10.1016/j.jaad.2015.12.010. Epub 2016 Mar 3 [PubMed PMID: 26947448]
Level 2 (mid-level) evidenceBrauer JA, Reddy KK, Anolik R, Weiss ET, Karen JK, Hale EK, Brightman LA, Bernstein L, Geronemus RG. Successful and rapid treatment of blue and green tattoo pigment with a novel picosecond laser. Archives of dermatology. 2012 Jul:148(7):820-3. doi: 10.1001/archdermatol.2012.901. Epub [PubMed PMID: 22801616]
Ross V, Naseef G, Lin G, Kelly M, Michaud N, Flotte TJ, Raythen J, Anderson RR. Comparison of responses of tattoos to picosecond and nanosecond Q-switched neodymium: YAG lasers. Archives of dermatology. 1998 Feb:134(2):167-71 [PubMed PMID: 9487208]
Mysore V, Anitha B, Hosthota A. Successful treatment of laser induced hypopigmentation with narrowband ultraviolet B targeted phototherapy. Journal of cutaneous and aesthetic surgery. 2013 Apr:6(2):117-9. doi: 10.4103/0974-2077.112677. Epub [PubMed PMID: 24023438]
Level 3 (low-level) evidenceMorlock R, Morlock A. Think Before You Ink: Perception, Prevalence, and Correlates of Tattooing and Tattoo Regret in US Adults. Cureus. 2023 Nov:15(11):e48167. doi: 10.7759/cureus.48167. Epub 2023 Nov 2 [PubMed PMID: 38046700]
Sepehri M, Jørgensen B. Surgical Treatment of Tattoo Complications. Current problems in dermatology. 2017:52():82-93. doi: 10.1159/000450808. Epub 2017 Mar 13 [PubMed PMID: 28288468]
Serup J, Bäumler W. Guide to Treatment of Tattoo Complications and Tattoo Removal. Current problems in dermatology. 2017:52():132-138. doi: 10.1159/000452966. Epub 2017 Mar 10 [PubMed PMID: 28288463]