Introduction
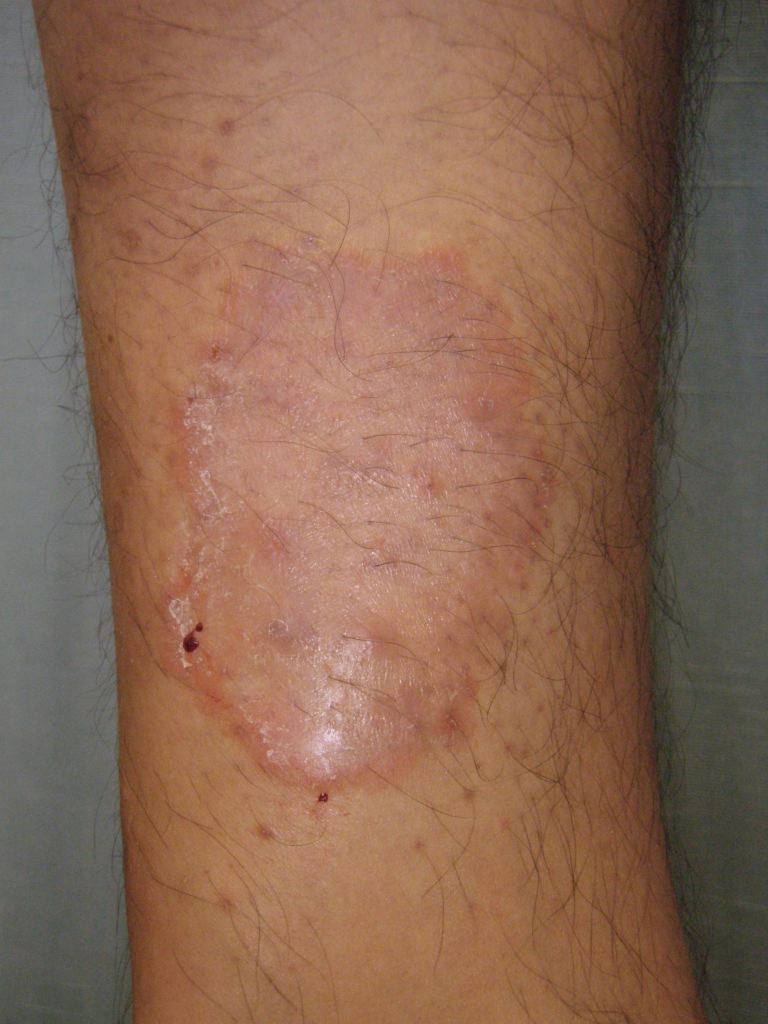
Tinea corporis is a superficial fungal skin infection of the body caused by dermatophytes (see Image. Tinea Corporis of the Forearm). This condition is prevalent worldwide, with lesions involving the trunk, neck, arms, and legs. There are different names for dermatophyte infections that affect various areas of the body. For instance, scalp involvement is called tinea capitis[1]. In contrast, infections of the face, hands, groin, and feet are referred to as tinea faciei,[2] tinea manuum,[3] tinea cruris, and tinea pedis, respectively.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
The ability of dermatophytes to attach to the keratinized tissue of the skin forms the basis for dermatophytoses, also termed superficial fungal skin infections.[4] The dermatophytes responsible for tinea corporis belong to the genera Trichophyton, Epidermophyton, and Microsporum. Over the past 70 years, Trichophyton rubrum has been the most common species to cause dermatophyte infections. T rubrum accounts for 80% to 90% of the pathogenic strains.[5] Other common isolates include T mentagrophytes and Microsporum audouinii. Direct skin contact with soil, animals, or other humans typically leads to infection.
In some cases, the most common etiologic species depends on the mode of transmission. Tinea corporis caused by T tonsurans often results from direct contact with a patient with tinea capitis. In the United States and the United Kingdom, T tonsurans is the most common causative agent of tinea capitis.[6][7] This species is also frequently identified in cases of tinea corporis gladiatorum, which typically occurs in athletes with extensive direct skin-to-skin contact, such as wrestlers.[8] Patients with tinea corporis who have close contact with cats or dogs are commonly infected with M canis.
Epidemiology
Tinea corporis is highly prevalent worldwide. Dermatophytes are the most prevalent agents of superficial fungal infections. Excessive heat, high relative humidity, and fitted clothing have correlations to more severe and frequent disease.[9]
Specific populations, such as children, are more predisposed to tinea corporis. [10] Tinea capitis and tinea corporis are the most common dermatophytic infections in prepubertal children.[11] Pediatric patients are also more likely to contract zoophilic infections, which are transmitted through contact with animals, such as cats and dogs. Individuals with compromised immune systems are not only more vulnerable to tinea corporis but also have an increased risk of developing Majocchi granuloma, a form of tinea corporis folliculitis that invades the deep dermal layers, unlike the superficial involvement observed in typical tinea corporis.[12]
Pathophysiology
Susceptibility to fungal infections varies among individuals, with familial and genetic predispositions potentially linked to specific defects in innate and adaptive immunity. A deficiency in defensin β4 may predispose patients to all dermatophytes. Additional risk factors include underlying conditions, such as diabetes mellitus, lymphomas, immunocompromised states, Cushing syndrome, excessive sweating, and advanced age. Current evidence suggests that the control of dermatophytosis primarily depends on a cell-mediated immune response.
Histopathology
Skin scrapings are subjected to microscopic examination after a 10% to 20% potassium hydroxide (KOH) solution is applied. Gentle heating enhances the preparation by dissolving keratin, highlighting the dermatophyte. Under the microscope, septate, branching, and long, narrow hyphae without constrictions can be visualized.
History and Physical
Patients commonly report an itchy, red rash that typically appears on exposed areas of the neck, trunk, or extremities. Physical examination reveals one or more circular or ovoid lesions, often presenting as patches or plaques. These annular lesions show sharp margins with a raised, erythematous, scaly edge, sometimes containing vesicles. The degree of inflammation varies. The lesions expand centrifugally, leaving central clearing with mild residual scaling. This characteristic ring appearance gives rise to the term ringworm.
Evaluation
Tinea corporis is typically diagnosed based on a detailed history and a thorough physical examination. Diagnostic tests can confirm the condition when needed. Microscopic evaluation of skin scrapings with a KOH preparation often reveals septate, branching, long, narrow hyphae. However, false negatives occur in up to 15% of cases when relying solely on KOH preparations.[13]
Fungal culture is another reliable method for confirming the diagnosis. Although fungal cultures can provide definitive identification, they require time for growth. Cultures typically show growth within 5 days, though some species may take up to 4 weeks. A sample is considered to have no growth after at least 4 weeks of lack of fungal colony development. The most commonly used isolation medium is Sabouraud dextrose agar (1% glucose, 4% mycological peptone, water). Identification involves analyzing the morphology, pigmentation, and surface topography of the culture sample.
Performing antifungal susceptibility testing on cultured organisms can help determine the most effective treatment regimen. This step is especially important for cases that are refractory to initial therapy, as it ensures the use of the most appropriate antifungal agent.
Dermoscopy may be used to identify characteristic features of tinea infections.[14] Research has identified 20 dermoscopic features in tinea capitis, 13 in tinea corporis, and 12 in tinea cruris. The most common dermoscopic feature in tinea capitis was corkscrew hairs, observed in 49 out of 110 patients.[15][16]
Treatment / Management
The treatment of dermatophyte infections typically involves topical or oral antifungal agents. The choice between these formulations depends on various factors, such as the severity, location, and extent of the infection; patient comorbidities; and response to previous treatments.
Localized tinea corporis typically improves with topical therapy, applied once or twice daily for 2 to 3 weeks. The endpoint of therapy is the clinical resolution of symptoms. In general, topical nystatin is ineffective for treating tinea corporis.
Recommended topical regimens include one of the following:
- Clotrimazole: 1% cream/ointment/solution applied topically twice daily
- Ketoconazole: 2% cream/shampoo/gel/foam applied once daily
- Miconazole: 2% cream/ointment/solution/lotion/powder applied twice daily
- Naftifine: 1% cream applied once daily or 1% or 2% gel applied twice daily
- Terbinafine: 1% cream/gel/spray solution applied once or twice daily
Oral therapy is necessary in cases involving more widespread infection or failed topical treatment. Oral terbinafine or itraconazole is typically the preferred first-line treatment and is expected to clear the condition in about 2 to 3 weeks.
Recommended oral regimens for adults include one of the following:
- Terbinafine: 250 mg orally once daily for 2 weeks
- Itraconazole: 100 mg once daily for 2 weeks or 200 mg once daily for 1 week; capsules must be taken with food
- Fluconazole: 150 to 200 mg once weekly or 50 to 100 mg/day for up to 4 weeks
- Griseofulvin: 500 to 1000 mg once daily for 2 to 4 weeks
Recently, trials have shown that tinea corporis caused by terbinafine-resistant T rubrum can be successfully treated with fosravuconazole.[17] In other cases of drug resistance, antifungal susceptibility testing is essential to guide treatment choice and ensure the use of the most effective agent.
Differential Diagnosis
Several diseases in the differential diagnosis can mimic the appearance of tinea corporis, often presenting with annular lesions. Cases that do not respond to antifungal treatment or have a negative KOH microscopic examination should prompt further investigation. Clinicians must also consider more serious conditions, especially in cases with extensive skin involvement or severe disease.
Other common conditions that may present similarly to tinea corporis include nummular eczema, erythema annulare centrifugum, tinea versicolor, cutaneous candidiasis, subacute cutaneous lupus erythematosus, pityriasis rosea, contact dermatitis, atopic dermatitis, seborrheic dermatitis, and psoriasis. Severe diseases that must be ruled out include secondary syphilis, mycosis fungoides, and parapsoriasis.
Prognosis
The prognosis for tinea corporis is generally excellent with appropriate treatment. Most localized cases respond well to topical antifungal agents within 2 to 4 weeks, especially when underlying predisposing factors are effectively addressed. Systemic antifungal therapy is effective in more extensive or refractory cases, with a high success rate when adherence is maintained. Recurrence can occur, particularly in the presence of persistent risk factors, such as immunosuppression, untreated tinea pedis or onychomycosis, and poor hygiene practices. Chronic or recurrent cases may require longer treatment courses or prophylactic measures. Delayed treatment or misdiagnosis can lead to atypical presentations or secondary bacterial infections, potentially complicating the clinical course.
Complications
Complications of dermatophytic infections are rare. One such complication is Majocchi granuloma, a condition where the dermatophyte invades through a follicle and advances deeper into the dermis or subcutaneous tissue. Minor skin trauma, such as shaving, can predispose patients to Majocchi granuloma. Lesions typically involve hair follicles and present as erythematous nodules or papules, which may progress to abscesses. Oral antifungals, such as terbinafine at a dosage of 250 mg once daily for 2 to 4 weeks, are the recommended treatment for this condition.
Deterrence and Patient Education
Education is paramount in preventing tinea corporis. Patients should be encouraged to wear light, loose-fitting clothing and keep the skin clean and dry to reduce the risk of developing the infection. Patients should also be advised to avoid sharing personal items, such as towels, clothing, or combs, to prevent the spread of tinea corporis. Clothing and bedding should be washed regularly in hot water, and direct contact with infected individuals or animals should be avoided. In addition, compliance with topical antifungal treatment is essential, although results are not immediate. Patients should be reminded that symptom resolution may take weeks, even with proper treatment.
Individuals with suppressed immunity should be closely monitored for tinea corporis, as they may be more susceptible to infections or develop more severe cases. Early diagnosis and treatment are crucial to prevent complications and promote faster recovery in this population.
Pearls and Other Issues
Hepatitis is a proven complication of ketoconazole, necessitating a baseline liver panel before initiating oral antifungals, particularly azoles. Terbinafine has been associated with a lupus-like reaction and should be used with caution in patients with systemic lupus erythematosus. Although allergic contact dermatitis to topical antifungals is rare, irritant effects may still occur.
Enhancing Healthcare Team Outcomes
Tinea corporis can be diagnosed through a clinical evaluation, which includes obtaining a history and performing a physical examination. In cases with an atypical appearance, further testing, such as a KOH test or fungal culture, should be considered.
Upon confirming the diagnosis of tinea corporis, the standard treatment involves topical antifungals. Due to potential adverse effects and reactions from systemic therapy, topical treatment is generally preferred over systemic therapy.
Tinea corporis management requires an interprofessional team approach involving clinicians, specialists, specialty-trained nurses, and pharmacists collaborating to achieve optimal patient outcomes. In most cases, clinicians diagnose the condition and prescribe treatment. Pharmacists verify the antifungal agent's coverage and dosing and communicate any concerns with the nurse or clinician. Nurses and pharmacists should ensure that baseline liver function tests are conducted and report any missing tests to the prescriber.
Pharmacists should also check for potential drug interactions or other medications that could contribute to hepatotoxicity, especially given the possible add-on effects of oral antifungal agents. If concerns arise, pharmacists should alert the nurse or prescriber to make appropriate adjustments to the therapeutic regimen. In addition, pharmacists can assess for drug-drug interactions, particularly with azole antifungals. Nurses and pharmacists should verify patient compliance and provide counseling on medication usage or dosing, reporting any issues to the prescribing clinician to facilitate necessary adjustments based on the patient's needs.
Media
(Click Image to Enlarge)
References
Heath CR, Usatine RP. Tinea Capitis. Cutis. 2022 Oct:110(4):226-227. doi: 10.12788/cutis.0630. Epub [PubMed PMID: 36446098]
Pei Y, Zhang LL, Liu ZH. Tinea Faciei. The Journal of pediatrics. 2022 Nov:250():108-109. doi: 10.1016/j.jpeds.2022.07.007. Epub 2022 Jul 11 [PubMed PMID: 35835226]
Córdoba García-Rayo M, González DV, Jiménez Briones L, Medrano Martínez N. Tinea manuum. Medicina clinica. 2024 Sep 27:163(6):e67. doi: 10.1016/j.medcli.2023.12.025. Epub 2024 Mar 7 [PubMed PMID: 38458958]
Aly R. Ecology and epidemiology of dermatophyte infections. Journal of the American Academy of Dermatology. 1994 Sep:31(3 Pt 2):S21-5 [PubMed PMID: 8077503]
Level 3 (low-level) evidenceSeebacher C, Bouchara JP, Mignon B. Updates on the epidemiology of dermatophyte infections. Mycopathologia. 2008 Nov-Dec:166(5-6):335-52. doi: 10.1007/s11046-008-9100-9. Epub 2008 May 14 [PubMed PMID: 18478365]
Level 3 (low-level) evidenceMirmirani P, Tucker LY. Epidemiologic trends in pediatric tinea capitis: a population-based study from Kaiser Permanente Northern California. Journal of the American Academy of Dermatology. 2013 Dec:69(6):916-21. doi: 10.1016/j.jaad.2013.08.031. Epub 2013 Oct 3 [PubMed PMID: 24094452]
Level 2 (mid-level) evidenceFuller LC, Child FC, Midgley G, Higgins EM. Scalp ringworm in south-east London and an analysis of a cohort of patients from a paediatric dermatology department. The British journal of dermatology. 2003 May:148(5):985-8 [PubMed PMID: 12786830]
Adams BB. Tinea corporis gladiatorum. Journal of the American Academy of Dermatology. 2002 Aug:47(2):286-90 [PubMed PMID: 12140477]
Taplin D. Dermatophytosis in Vietnam. Cutis. 2001 May:67(5 Suppl):19-20 [PubMed PMID: 11398256]
Vargas-Navia N, Ayala Monroy GA, Franco Rúa C, Malagón Caicedo JP, Rojas Hernández JP. [Tinea capitis in children]. Revista chilena de pediatria. 2020 Oct:91(5):773-783. doi: 10.32641/rchped.vi91i5.1345. Epub [PubMed PMID: 33399644]
Ely JW, Rosenfeld S, Seabury Stone M. Diagnosis and management of tinea infections. American family physician. 2014 Nov 15:90(10):702-10 [PubMed PMID: 25403034]
Elgart ML. Tinea incognito: an update on Majocchi granuloma. Dermatologic clinics. 1996 Jan:14(1):51-55 [PubMed PMID: 8821157]
Panasiti V, Borroni RG, Devirgiliis V, Rossi M, Fabbrizio L, Masciangelo R, Bottoni U, Calvieri S. Comparison of diagnostic methods in the diagnosis of dermatomycoses and onychomycoses. Mycoses. 2006 Jan:49(1):26-9 [PubMed PMID: 16367815]
Dhaille F, Dillies AS, Dessirier F, Reygagne P, Diouf M, Baltazard T, Lombart F, Hébert V, Chopinaud M, Verneuil L, Becquart C, Delaporte E, Lok C, Chaby G. A single typical trichoscopic feature is predictive of tinea capitis: a prospective multicentre study. The British journal of dermatology. 2019 Nov:181(5):1046-1051. doi: 10.1111/bjd.17866. Epub 2019 Apr 29 [PubMed PMID: 30844082]
Babba ZI, Shehu MY, Ukonu BA, Ibekwe PU. Dermoscopic Features seen in Tinea Capitis, Tinea Corporis and Tinea Cruris. West African journal of medicine. 2023 May 27:40(5):463-468 [PubMed PMID: 37245212]
Arrazola-Guerrero J, Isa-Isa R, Torres-Guerrero E, Arenas R. [Tinea capitis. Dermoscopic findings in 37 patients]. Revista iberoamericana de micologia. 2015 Oct-Dec:32(4):242-6. doi: 10.1016/j.riam.2014.09.002. Epub 2015 Jan 6 [PubMed PMID: 25728878]
Kitauchi Y, Kumagai Y, Inoue-Masuda Y, Sugiura M, Sato T, Yaguchi T, Yokoyama T. Tinea corporis caused by terbinafine-resistant Trichophyton rubrum successfully treated with fosravuconazole. The Journal of dermatology. 2021 Jul:48(7):e329-e330. doi: 10.1111/1346-8138.15900. Epub 2021 Apr 16 [PubMed PMID: 33860550]