Anatomy, Shoulder and Upper Limb, Glenohumeral Joint
Anatomy, Shoulder and Upper Limb, Glenohumeral Joint
Introduction
The glenohumeral joint is a ball-and-socket joint structurally and a diarthrodial, multiaxial joint functionally.[1] This joint is the shoulder girdle's major articulation, uniting the humeral head with the scapula's glenoid cavity.[2] Minor shoulder articulations include the sternoclavicular, acromioclavicular, and scapulothoracic joints.[3][4] The glenohumeral joint exhibits the highest degree of mobility among all human joints. Static and dynamic stabilizing structures allow for a wide range of motion in multiple body planes that predispose the joint to injury (see Image. Left Shoulder Anatomy).
The glenohumeral joint is inherently unstable, making it prone to dislocations, rotator cuff tears, and degenerative conditions such as osteoarthritis. Clinically, management ranges from conservative rehabilitation to surgical interventions, including arthroscopic repair for soft tissue injuries and total shoulder arthroplasty for severe joint degeneration. Surgical approaches must balance restoring stability with preserving range of motion to optimize functional outcomes. Understanding the anatomy and function of the glenohumeral joint is essential for managing various upper limb pathologies.
Structure and Function
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Structure and Function
The glenohumeral joint is a ball-and-socket joint of the upper limb formed by the dynamic articulation between the scapula's glenoid cavity and the humeral head. Articular cartilage covers the articulating surfaces of these bones. The glenoid cavity is a shallow osseous structure deepened by a fibrocartilaginous rim, the glenoid labrum, which spans the vault’s osseous periphery. The labrum is continuous with the tendon of the long head of the biceps brachii (long head of biceps tendon or LHBT) at its superior aspect. The loose joint capsule and the humeral head’s disproportionate size relative to the shallow glenoid fossa (a 4:1 surface area ratio) contribute to the shoulder joint’s high mobility and susceptibility to dislocation.
The glenohumeral joint capsule is a fibrous sheath that forms a continuous support structure around the articulating elements, encircling the region from the anatomical neck of the humerus to the rim of the glenoid fossa. Within this capsule, the capsulolabral complexes contain distinct thickened bands, known as the glenohumeral ligaments, first described in 1829. These ligaments become taut at varying degrees of abduction and humeral rotation, unlike traditional ligaments that carry a pure tensile force along their length.[5][6] A synovial membrane also lines the joint capsule's inner surface, secreting synovial fluid to minimize friction between the articular surfaces.[7]
Multiple synovial bursae help reduce friction within the glenohumeral joint by cushioning between joint structures such as tendons. The shoulder bursae include the subacromial (subdeltoid), subcoracoid, and subscapular bursae.
The subacromial bursa lies between the deltoid muscle and the joint capsule in the superolateral aspect of the glenohumeral joint, superficial to the supraspinatus tendon. This bursa reduces friction underneath the deltoid muscle, allowing a greater range of motion. The subacromial bursa does not usually communicate with the shoulder joint. The subscapular bursa lies between the subscapularis tendon and the capsule, reducing frictional damage to the subscapularis muscle during internal shoulder rotation. The subcoracoid bursa is situated between the coracoid process and the subscapularis. The subacromial and subscapular bursae are clinically significant due to their vulnerability to injury.
Shoulder ligaments include the glenohumeral, coracoglenoid, coracohumeral, transverse humeral, coracoacromial, coracoclavicular, and acromioclavicular ligaments. The glenohumeral ligaments are composed of the superior, middle, and inferior ligaments. These fibrous structures are intrinsic to the glenohumeral region, reinforcing the glenohumeral capsule and preventing anterior shoulder dislocation. The glenohumeral ligaments serve as the primary stabilizers of the joint.
The coracoglenoid ligament is a component of the anterior limb of the superior glenohumeral ligament. This ligament originates from the middle of the coracoid process and inserts posterior to the supraglenoid tubercle, covering the superior glenoid rim, labrum, and LHBT. This ligament contributes to the anterosuperior stabilization of the shoulder joint.[8]
The coracohumeral ligament is an intrinsic band that supports the superior aspect of the glenohumeral joint capsule. This dense fibrous structure extends from the base of the coracoid process to the greater and lesser tuberosities. The ligament is thin and broad at its origin, measuring about 2 cm in diameter at the coracoid base. Laterally, this ligament separates into 2 distinct bands that envelop the LHBT at the proximal end of the bicipital groove.
The transverse humeral ligament secures the LHBT within the bicipital groove, passing between the greater and lesser tuberosities over the tendon sheath. Research suggests the absence of a distinct, separate transverse humeral ligament. Instead, the roof of the intertubercular groove comprises fibers from the subscapularis tendon, with contributions from the supraspinatus tendon and the coracohumeral ligament. Additionally, the transverse humeral ligament is closely associated with the biceps pulley.
The coracoacromial ligament is a robust, fibrous triangular band that forms a crucial part of the coracoacromial arch. This osteoligamentous arch is extrinsic to the glenohumeral region, shielding the humeral head and rotator cuff tendons from trauma. This ligament contributes to the roof of the glenohumeral joint, limiting the space available to the rotator cuff tendons, subacromial subdeltoid bursa, and the LHBT. Dysfunction or compression of these structures due to coracoacromial ligament abnormalities can lead to subacromial impingement syndrome and subacromial bursitis.
The coracoclavicular ligament consists of the conoid and trapezoid ligaments and spans from the coracoid process to the clavicle. This ligament preserves vertical stability at the acromioclavicular joint, preventing superior clavicular dislocation. Strong forces causing acromioclavicular joint injuries can rupture this ligament or its components. The acromioclavicular ligament comprises superior and inferior parts. The superior ligament spans from the upper acromion to the clavicle's edge, stabilizing the joint horizontally. The inferior acromioclavicular ligament is thinner than its superior counterpart and covers the lower joint portion, attaching to the adjoining surfaces of both bones.[9][10] Acromioclavicular joint injuries often present with glenohumeral damage due to the proximity of these structures.[11]
Static stabilizers of the glenohumeral joint include osseous articular anatomy, joint congruity, the glenoid labrum, glenohumeral ligaments, the joint capsule, and negative intraarticular pressure. Dynamic stability relies on the LHBT, rotator cuff muscles, rotator interval, and periscapular muscles.
Soft-Tissue Pulley System and the Long Head of the Biceps Tendon
The subscapularis consists of superficial and deep fibers that surround the bicipital groove, forming its "roof" and "floor," respectively. These fibers merge with those from the supraspinatus and the superior glenohumeral ligament/coracohumeral ligament complex. These structures attach intimately at the lesser tuberosity, forming the proximal and medial aspects of the pulley system, with soft tissue extensions enveloping the LHBT within the bicipital groove. The LHBT exits the groove and takes a 30º to 40º turn as it heads toward the supraglenoid tubercle and glenoid labrum. Thus, the proximal soft tissue elements of the groove play a critical role in maintaining the overall stability of the biceps complex.[12][13]
Glenohumeral Joint Motion
The glenohumeral joint permits a vast range of motion across multiple planes. Understanding the contribution of various muscles to these movements is essential for differentiating shoulder pathologies.[14]
Flexion moves the upper limb anteriorly in the sagittal plane. The typical range of motion is 180º. The shoulder's main flexors are the anterior deltoid, coracobrachialis, and pectoralis major. The biceps brachii weakly assists in this action. Extension displaces the upper limb posteriorly in the sagittal plane. The normal motion range is 45º to 60º. The shoulder's principal extensors are the posterior deltoid, latissimus dorsi, and teres major.
Internal rotation involves limb rotation toward the midline along a vertical axis. The normal range of motion is 70º to 90º. The shoulder's internal rotators are the subscapularis, pectoralis major, latissimus dorsi, teres major, and the anterior deltoid. External rotation entails limb rotation away from the midline along a vertical axis. The normal range of motion is 90º. The infraspinatus and teres minor are chiefly responsible for this action.
Adduction moves the upper limb toward the midline in the coronal plane, mainly driven by the latissimus dorsi, teres major, and pectoralis major. Abduction displaces the upper limb away from the midline in the coronal plane. The normal range of motion is 150º. The supraspinatus abducts the shoulder for the first 0º to 15º.[15] The deltoid's middle fibers abduct the shoulder from 15º to 90º.[16] Scapular rotation from activating the trapezius and serratus anterior enables further abduction beyond 90º.
Rotator Cable and Rotator Interval
The rotator cable and interval are crucial joint stabilizers that have generated tremendous interest in recent years. Although plain radiographs cannot visualize these structures, their pathologies are believed to contribute significantly to degenerative shoulder injuries.
The rotator cable originates from the coracohumeral ligament and divides into superficial and deep layers. This structure encircles the rotator cuff and inserts into the lesser and greater humeral tuberosities. The deeper layer forms a crescent-shaped configuration, extending posteriorly from the anterior insertion of the supraspinatus to the inferior border of the infraspinatus. This anatomical arrangement contributes significantly to shoulder stability. Research indicates that rotator cable thickness varies among individuals, with older shoulders tending to exhibit thicker cables, suggesting a shift toward greater reliance on this structure for superior rotator cuff stability with age.[17][18]
The rotator interval consists of anterior and posterior segments, though the anterior portion holds greater clinical relevance. This triangular space is bordered superiorly by the supraspinatus tendon, inferiorly by the subscapularis tendon, laterally by the coracohumeral ligament, and medially by the superior glenohumeral ligament. The rotator interval houses the LHBT, coracohumeral ligament, and superior glenohumeral ligament. This structure functions as a soft tissue restraint, securing the LHBT within the bicipital groove and preventing anteromedial subluxation during external rotation and anteroinferior subluxation during shoulder abduction. Additionally, the rotator interval restricts excessive inferior movement of the shoulder joint. Anatomical variations in this region may contribute to shoulder pathology.[19]
Embryology
Skeletal shoulder development involves both intramembranous and endochondral ossification. The clavicle forms through intramembranous ossification, where bone develops directly within the mesenchyme. The remaining shoulder structures arise via endochondral ossification.[20] The mesoderm germ layer gives rise to nearly all connective tissues within the musculoskeletal system, including the glenohumeral joint. Congenital musculoskeletal and limb anomalies, influenced by both genetic and environmental factors, represent a significant subset of developmental disorders.
Blood Supply and Lymphatics
The glenohumeral joint receives vascular supply from the posterior (PCHA) and anterior (ACHA) circumflex humeral arteries, both branches of the axillary artery. The PCHA contributes more significantly (64%) than the ACHA (34%) to the humeral head's blood supply. Distribution varies, with the PCHA perfusing the humeral head's lateral, superior, and inferior quadrants, while the ACHA primarily supplies a portion on the inferior aspect.[21][22] The arcuate artery extends from the ACHA's ascending branch and enters the bicipital groove. The subscapular artery, arising from the thyrocervical trunk, sends branches to the shoulder.[23] Veins accompanying these arteries drain the glenohumeral region.[24]
Most upper extremity lymphatic vessels drain toward the axilla. Axillary nodes are categorized into 5 groups based on location: pectoral, subscapular, humeral, central, and apical. Efferent vessels from the apical axillary nodes traverse the cervicoaxillary canal and merge to form the subclavian lymphatic trunk, which either drains into the right venous angle on the right or empties directly into the thoracic duct on the left. Assessing axillary lymph node involvement is vital for breast cancer staging. Disrupting lymphatic drainage can result in lymphedema, where subcutaneous lymph accumulation leads to painful upper limb swelling.[25]
Nerves
The suprascapular, lateral pectoral, and axillary nerves supply the glenohumeral joint. These nerves originate from the brachial plexus, a nerve network formed by the ventral rami of C5 to T1. Axillary nerve anatomy is critical, as it is close to the glenohumeral joint. The axillary nerve originates from the posterior cord of the brachial plexus, courses along the subscapularis to its inferior border, and travels closely along the inferior glenohumeral joint capsule. The nerve then transits posterior to the humerus, wraps around the surgical humeral neck alongside the PCHA, and enters the quadrangular space before running within the deep deltoid fascia.[26]
Muscles
The 4 muscles that constitute the rotator cuff are the supraspinatus, infraspinatus, subscapularis, and teres minor. The primary biomechanical function of the rotator cuff is to stabilize the glenohumeral joint by compressing the humeral head against the glenoid. The rotator cuff muscles thus act as the glenohumeral joint's dynamic stabilizers.[27][28] The LHBT also has a debated contribution to glenohumeral joint stability. Current consensus suggests that the LHBT's stabilizing role becomes more significant in the presence of rotator cuff dysfunction.[29]
The supraspinatus primarily abducts the shoulder and initiates the first 15° of abduction. The infraspinatus and teres minor contribute to external rotation, while the subscapularis facilitates internal rotation. The suprascapular nerve innervates the supraspinatus and infraspinatus muscles. The axillary nerve supplies the teres minor. The subscapular nerve innervates the subscapularis.
Physiologic Variants
Glenohumeral joint variations may arise from differences in glenoid cavity and humeral head shape and size. The glenoid cavity may be pear-shaped, oval, or inverted comma-shaped. The pear shape is the most common, while the inverted comma shape is the least prevalent. The oval shape provides the greatest stability, whereas the inverted comma shape is the least stable. These anatomical variations influence prosthetic design after shoulder arthroplasty and affect glenohumeral movement in sports such as javelin throwing and tennis.[30]
Humeral head shape variations influence the LHBT reflection pulley's movement and stability. Humeral head shape may be flat, convex, spiculated, or mixed. Flat humeral heads are prevalent in men and younger individuals, while convex ones are more common among women and older individuals. The mixed type occurs least frequently.[31]
Surgical Considerations
Shoulder osteoarthritis narrows the glenohumeral joint space due to joint capsule thickening and degeneration of the articular cartilage and subchondral bone. Osteoarthritis-related shoulder pain is a common and debilitating condition. Nonsurgical treatments include oral analgesics, intraarticular injections, physical therapy, and acupuncture, though evidence supporting their effectiveness in shoulder osteoarthritis is inconclusive. Unresponsiveness to conservative measures warrants surgical intervention.
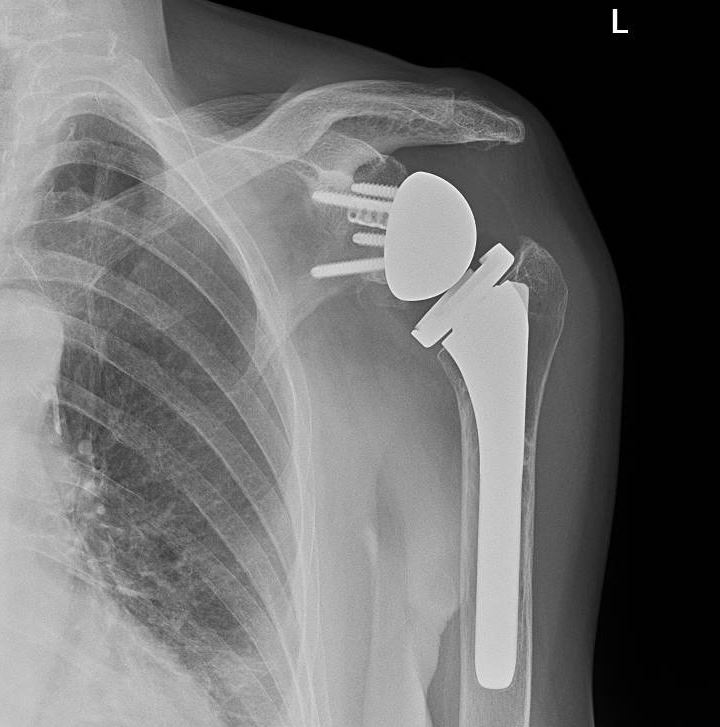
Joint replacement surgery for shoulder osteoarthritis involves removing damaged bone and cartilage and releasing tight soft tissues contributing to contractures. Prosthetic materials replace the resected structures to restore shoulder joint anatomy and function. This procedure is the primary surgical treatment for shoulder osteoarthritis and may entail replacing only the humeral head (hemiarthroplasty) or both the humeral head and glenoid (total shoulder replacement). Newer techniques, particularly reverse total shoulder replacement, are gaining popularity, especially among younger patients and those with less advanced disease (see Image. Reverse Total Shoulder Arthroplasty).[32]
Clinical Significance
Shoulder Dislocations
The glenohumeral joint is by far the most frequently dislocated joint of the body, accounting for up to 45% of dislocations. Anterior dislocation comprises 96% of cases and is often the result of a force directed to the shoulder joint while the arm is abducted and externally rotated. Posterior dislocation is the 2nd most common, accounting for 2% to 4% of cases. Posterior dislocations usually arise from indirect mechanisms, such as electric shock or convulsions, causing contraction of the relatively stronger internal shoulder rotators, the latissimus dorsi, pectoralis major, and subscapularis.
The incidence of glenohumeral joint dislocation is approximately 17 per 100,000 annually, with peak occurrences among men aged 21 to 30 and women aged 61 to 80. Treatment typically involves analgesics and closed reduction, with some patients requiring subsequent surgical correction, especially those with recurrent shoulder dislocations from concurrent soft tissue injuries.[33] The axillary nerve, which wraps around the humeral surgical neck, can sustain damage during dislocation or reduction attempts. Axillary nerve injury may lead to deltoid paralysis and loss of sensation over the lateral shoulder.
Hill-Sachs lesions result from impaction fractures of the posterolateral humeral head against the anteroinferior glenoid. Bankart lesions stem from the detachment of the anteroinferior labrum with or without an avulsion fracture. Anterior dislocation can cause both conditions. The recurrence rate for glenohumeral joint dislocation averages 50%, with a higher risk in individuals who experience their first dislocation at a younger age.[34]
Adhesive Capsulitis
Adhesive capsulitis is characterized by glenohumeral capsule inflammation and stiffness, leading to significant motion restriction and chronic pain that typically worsens at night. The condition affects approximately 3% of the general population and is more common in adult women aged 40 to 70.[35] Risk factors include diabetes mellitus, connective tissue diseases, thyroid disease, and heart disease, with highly active antiretroviral therapies also implicated.[36]
Management includes physical and occupational therapy, analgesic medications, intraarticular steroid injections, and, in some cases, surgical intervention. Surgical options may involve manipulation under general anesthesia to disrupt joint adhesions and scar tissue. Most individuals eventually regain around 90% of their shoulder range of motion.
Rotator Cuff Injuries
The rotator cuff tendons are often injured due to their crucial role in stabilizing the glenohumeral joint. Rotator cuff conditions, including subacromial bursitis, tendinitis, impingement, and tears, are the primary source of shoulder pain in primary care settings.[37] Patients with impingements or subacromial bursitis often experience pain during overhead activities. Most cases improve with physical therapy, but persistent symptoms warrant an evaluation by an orthopedic surgeon or sports medicine specialist. Rotator cuff tears are often associated with tendon degeneration or shoulder impingement and may be classified as chronic or acute, partial- or full-thickness.
Media
(Click Image to Enlarge)
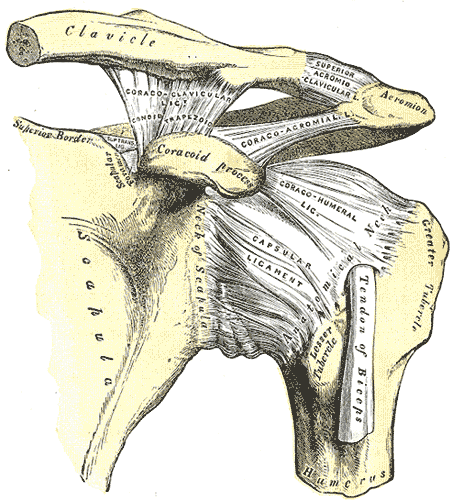
Left Shoulder Anatomy. This image shows the anatomic relationships between the clavicle, scapula, scapular neck, foramen, and superior border, coracoid process, acromion, greater and lesser humeral tubercles, humerus and anatomical neck, tendon of the biceps brachii long head, and the coracoclavicular (with the conoid and trapezoid), coracoacromial, superior acromioclavicular, coracohumeral, and capsular ligaments.
Henry Vandyke Carter, Public Domain, via Wikimedia Commons
(Click Image to Enlarge)
References
McCausland C, Sawyer E, Eovaldi BJ, Varacallo MA. Anatomy, Shoulder and Upper Limb, Shoulder Muscles. StatPearls. 2025 Jan:(): [PubMed PMID: 30521257]
Cowan PT, Mudreac A, Varacallo MA. Anatomy, Back, Scapula. StatPearls. 2025 Jan:(): [PubMed PMID: 30285370]
Epperson TN, Black AC, Varacallo MA. Anatomy, Shoulder and Upper Limb, Sternoclavicular Joint. StatPearls. 2025 Jan:(): [PubMed PMID: 30725943]
Mostafa E, Imonugo O, Varacallo MA. Anatomy, Shoulder and Upper Limb, Humerus. StatPearls. 2025 Jan:(): [PubMed PMID: 30521242]
Itoigawa Y, Itoi E. Anatomy of the capsulolabral complex and rotator interval related to glenohumeral instability. Knee surgery, sports traumatology, arthroscopy : official journal of the ESSKA. 2016 Feb:24(2):343-9. doi: 10.1007/s00167-015-3892-1. Epub 2015 Dec 24 [PubMed PMID: 26704796]
Burkart AC, Debski RE. Anatomy and function of the glenohumeral ligaments in anterior shoulder instability. Clinical orthopaedics and related research. 2002 Jul:(400):32-9 [PubMed PMID: 12072743]
Jahn S, Seror J, Klein J. Lubrication of Articular Cartilage. Annual review of biomedical engineering. 2016 Jul 11:18():235-58. doi: 10.1146/annurev-bioeng-081514-123305. Epub [PubMed PMID: 27420572]
Desai S, Patil NG, Kapoor T. Coracoid Process-A Hub of Shoulder Ligaments. The Indian journal of radiology & imaging. 2022 Mar:32(1):5-9. doi: 10.1055/s-0041-1741091. Epub 2022 Mar 17 [PubMed PMID: 35722651]
Kadi R, Milants A, Shahabpour M. Shoulder Anatomy and Normal Variants. Journal of the Belgian Society of Radiology. 2017 Dec 16:101(Suppl 2):3. doi: 10.5334/jbr-btr.1467. Epub 2017 Dec 16 [PubMed PMID: 30498801]
Filardi V. Stress distribution in the humerus during elevation of the arm and external abduction. Journal of orthopaedics. 2020 May-Jun:19():218-222. doi: 10.1016/j.jor.2020.02.003. Epub 2020 Feb 4 [PubMed PMID: 32071517]
Li X, Ma R, Bedi A, Dines DM, Altchek DW, Dines JS. Management of acromioclavicular joint injuries. The Journal of bone and joint surgery. American volume. 2014 Jan 1:96(1):73-84. doi: 10.2106/JBJS.L.00734. Epub [PubMed PMID: 24382728]
Varacallo MA, Seaman TJ, Mair SD. Biceps Tendon Dislocation and Instability. StatPearls. 2025 Jan:(): [PubMed PMID: 30475566]
Tiwana MS, Charlick M, Varacallo MA. Anatomy, Shoulder and Upper Limb, Biceps Muscle. StatPearls. 2025 Jan:(): [PubMed PMID: 30137823]
Bakhsh W, Nicandri G. Anatomy and Physical Examination of the Shoulder. Sports medicine and arthroscopy review. 2018 Sep:26(3):e10-e22. doi: 10.1097/JSA.0000000000000202. Epub [PubMed PMID: 30059442]
Maruvada S, Madrazo-Ibarra A, Varacallo MA. Anatomy, Rotator Cuff. StatPearls. 2025 Jan:(): [PubMed PMID: 28722874]
Elzanie A, Varacallo MA. Anatomy, Shoulder and Upper Limb, Deltoid Muscle. StatPearls. 2025 Jan:(): [PubMed PMID: 30725741]
Huri G, Kaymakoglu M, Garbis N. Rotator cable and rotator interval: anatomy, biomechanics and clinical importance. EFORT open reviews. 2019 Feb:4(2):56-62. doi: 10.1302/2058-5241.4.170071. Epub 2019 Feb 20 [PubMed PMID: 30931149]
Yubran AP, Pesquera LC, Juan ELS, Saralegui FI, Canga AC, Camara AC, Valdivieso GM, Pisanti Lopez C. Rotator cuff tear patterns: MRI appearance and its surgical relevance. Insights into imaging. 2024 Feb 27:15(1):61. doi: 10.1186/s13244-024-01607-w. Epub 2024 Feb 27 [PubMed PMID: 38411840]
Thaker S, O'Connor P, Gupta H. Ultrasound evaluation of the rotator interval and adjoining tendons in shoulders with restricted movements: a technical note describing a simplified shoulder position. Journal of ultrasound. 2022 Mar:25(1):115-119. doi: 10.1007/s40477-020-00541-z. Epub 2021 Jan 27 [PubMed PMID: 33502663]
Hyland S, Charlick M, Varacallo MA. Anatomy, Shoulder and Upper Limb, Clavicle. StatPearls. 2025 Jan:(): [PubMed PMID: 30252246]
Keough N, Lorke DE. The humeral head: A review of the blood supply and possible link to osteonecrosis following rotator cuff repair. Journal of anatomy. 2021 Nov:239(5):973-982. doi: 10.1111/joa.13496. Epub 2021 Jun 23 [PubMed PMID: 34164802]
Pencle F, Varacallo MA. Proximal Humerus Fracture. StatPearls. 2025 Jan:(): [PubMed PMID: 29262220]
McClelland D, Paxinos A. The anatomy of the quadrilateral space with reference to quadrilateral space syndrome. Journal of shoulder and elbow surgery. 2008 Jan-Feb:17(1):162-4 [PubMed PMID: 17993281]
Alashkham A, Alraddadi A, Felts P, Soames R. Blood supply and vascularity of the glenoid labrum: Its clinical implications. Journal of orthopaedic surgery (Hong Kong). 2017 Sep-Dec:25(3):2309499017731632. doi: 10.1177/2309499017731632. Epub [PubMed PMID: 28920546]
Suami H, Koelmeyer L, Mackie H, Boyages J. Patterns of lymphatic drainage after axillary node dissection impact arm lymphoedema severity: A review of animal and clinical imaging studies. Surgical oncology. 2018 Dec:27(4):743-750. doi: 10.1016/j.suronc.2018.10.006. Epub 2018 Oct 12 [PubMed PMID: 30449502]
Level 3 (low-level) evidenceZurkiya O. Quadrilateral space syndrome. Cardiovascular diagnosis and therapy. 2021 Oct:11(5):1112-1117. doi: 10.21037/cdt-20-147. Epub [PubMed PMID: 34815962]
Varacallo MA, El Bitar Y, Mair SD. Rotator Cuff Tendonitis. StatPearls. 2025 Jan:(): [PubMed PMID: 30335303]
Varacallo MA, El Bitar Y, Sina RE, Mair SD. Rotator Cuff Syndrome. StatPearls. 2025 Jan:(): [PubMed PMID: 30285401]
Varacallo MA, Mair SD. Proximal Biceps Tendinitis and Tendinopathy. StatPearls. 2025 Jan:(): [PubMed PMID: 30422594]
Singh R. Surgical Anatomy of the Glenoid Cavity and Its Use in Shoulder Arthroplasty Among the North Indian Population. Cureus. 2020 Dec 6:12(12):e11940. doi: 10.7759/cureus.11940. Epub 2020 Dec 6 [PubMed PMID: 33425520]
Fischetti M, Stoppino LP, Petrera MR, Francavilla A, Vinci R, Zappia M, Macarini L. MRI morphological evaluation of humeral head bone profile inside region of the biceps pulley reflection. Skeletal radiology. 2022 Oct:51(10):2017-2025. doi: 10.1007/s00256-022-04056-y. Epub 2022 Apr 22 [PubMed PMID: 35460041]
Craig RS, Goodier H, Singh JA, Hopewell S, Rees JL. Shoulder replacement surgery for osteoarthritis and rotator cuff tear arthropathy. The Cochrane database of systematic reviews. 2020 Apr 21:4(4):CD012879. doi: 10.1002/14651858.CD012879.pub2. Epub 2020 Apr 21 [PubMed PMID: 32315453]
Level 1 (high-level) evidenceVezeridis PS, Ishmael CR, Jones KJ, Petrigliano FA. Glenohumeral Dislocation Arthropathy: Etiology, Diagnosis, and Management. The Journal of the American Academy of Orthopaedic Surgeons. 2019 Apr 1:27(7):227-235. doi: 10.5435/JAAOS-D-17-00056. Epub [PubMed PMID: 30278009]
Khatri K, Arora H, Chaudhary S, Goyal D. Meta-Analysis of Randomized Controlled Trials Involving Anterior Shoulder Instability. The open orthopaedics journal. 2018:12():411-418. doi: 10.2174/1874325001812010411. Epub 2018 Oct 25 [PubMed PMID: 30505371]
Level 1 (high-level) evidenceAllen GM. The diagnosis and management of shoulder pain. Journal of ultrasonography. 2018:18(74):234-239. doi: 10.15557/JoU.2018.0034. Epub [PubMed PMID: 30451406]
De Ponti A, Viganò MG, Taverna E, Sansone V. Adhesive capsulitis of the shoulder in human immunodeficiency virus-positive patients during highly active antiretroviral therapy. Journal of shoulder and elbow surgery. 2006 Mar-Apr:15(2):188-90 [PubMed PMID: 16517362]
Rosenfeld SB, Schroeder K, Watkins-Castillo SI. The Economic Burden of Musculoskeletal Disease in Children and Adolescents in the United States. Journal of pediatric orthopedics. 2018 Apr:38(4):e230-e236. doi: 10.1097/BPO.0000000000001131. Epub [PubMed PMID: 29401074]